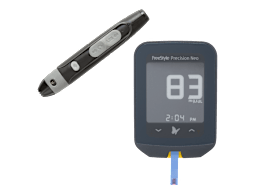
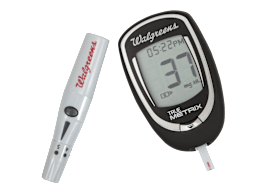
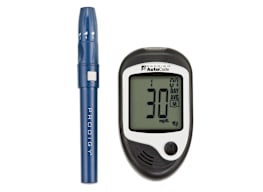
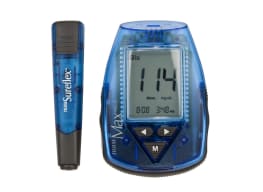
Blood Glucose Meter Buying Guide
Controlling your blood sugar, or blood glucose, level is key to managing diabetes. Accurate test results help people with diabetes adjust their diet, exercise routine, and treatment plan—which might help prevent complications and reduce the risk of seizures, kidney disease, nerve damage, and blindness.
Anyone with diabetes can benefit from testing. Blood glucose monitoring can be important for those taking insulin or other diabetes medications, for women with gestational diabetes (diagnosed during pregnancy), and for people having difficulty controlling their diabetes.
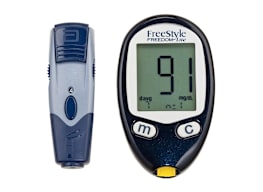
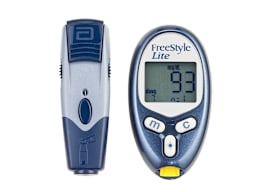
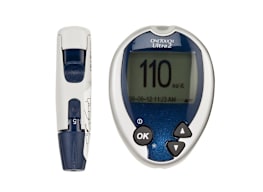
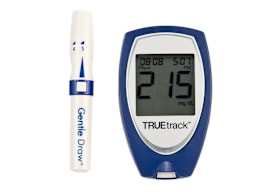
Today’s blood glucose meters are smaller, faster, and more accurate than older models, and they come with more features. We tested 18 models priced between $15 and $30. Use our guide to help you find the best monitor for your needs.
Choosing a Blood Glucose Meter
All glucose monitors work in a similar way, but some have features and options that might better suit your particular needs. Talk with your doctor or diabetes educator about which model matches your monitoring requirements, lifestyle, and budget.
Cost
Don’t look at the retail price of the meters alone. What makes blood glucose monitoring expensive is the test strips, which you might use many times a day. At $18 to $184 per 100 test strips, the cost can add up to about $265 to $2,685 per year for people who test four times a day. Replacement lancets are another expense to consider.
Insurance
Medicare covers some diabetes-related supplies, and private insurance might cover some of the cost. See whether there are certain brands of meters and test strips that your insurance covers. Find out how many test strips, if any, are covered per month. Your strip coverage may depend, for example, on whether you use insulin.
Automatic Coding
Blood glucose meters need to be calibrated to each batch of test strips. Some require you to enter a code or download an app so that you can scan the codes with a smartphone. Entering this information incorrectly can result in inaccurate results. Other models use a removable code chip to calibrate the meter to each batch of strips.
Data Storage
The most convenient blood glucose meters store at least 360 test results. Some also track the average of your readings over seven, 14, or 30 days to give you a view of your overall blood sugar control. If you check your blood glucose frequently, consider buying a model with more memory.
Test Time
The difference of a few seconds might not seem like much, but when you’re using a meter three to five times a day, a longer test time can be a nuisance. Our panelists found that 5 seconds or less was desirable.
Markers and Flags
These features allow you to note whether a reading was taken before or after a meal or exercise.
Unit Size
If you need to test while you’re on the go, look for a compact meter. Some larger models store multiple strips so that you don’t need to load one for each test, but our panelists found them to be bulky. Still, these models might make home testing more convenient, especially for people with dexterity or vision difficulties. Most models require a watch-style or medical battery, but consider getting a model that uses AAA batteries, which might be easier to replace.
Blood-Sample Size
Today’s blood glucose meters require smaller blood samples than those from years past. That makes testing less painful. If you’re sensitive to lancing, look for a meter that requires less than 1 microliter of blood.
How We Test Blood Glucose Meters
Our accuracy and repeatability tests of glucose monitoring systems are patterned after ISO standard 15197. That’s a set of guidelines from the International Organization for Standardization outlining requirements for the accuracy of blood glucose monitors used for self-testing by people with diabetes mellitus. Our ratings allow you to compare the accuracy of various models above and beyond current guidelines. All models we tested are well within current accuracy regulations, but only those with a Very Good or Excellent score earned our recommendation.
Secrets to Diabetes Management
Our survey found that simple approaches are often the best.