Your Questions About COVID-19 Booster Shots, Answered
New booster shots targeting omicron subvariants are recommended for people 5 and older.
Booster shots against the coronavirus that causes COVID-19 have been available and recommended for fully vaccinated adults since November 2021. As the omicron wave surged, the Food and Drug Administration and the Centers for Disease Control and Prevention gradually expanded access to boosters to younger populations (kids 5 and older have been eligible since May) and also authorized a second booster dose for people 50 and older or who have medical conditions that put them at greater risk for severe disease.
Those boosters were basically more of the same—additional doses of the vaccines that were already widely available. But that has changed.
Over the summer, the FDA’s vaccine advisory panel called on vaccine manufacturers to reformulate their products to target currently circulating omicron subvariants, which are quite different from the original strain of the coronavirus that vaccines and boosters had been designed to target.
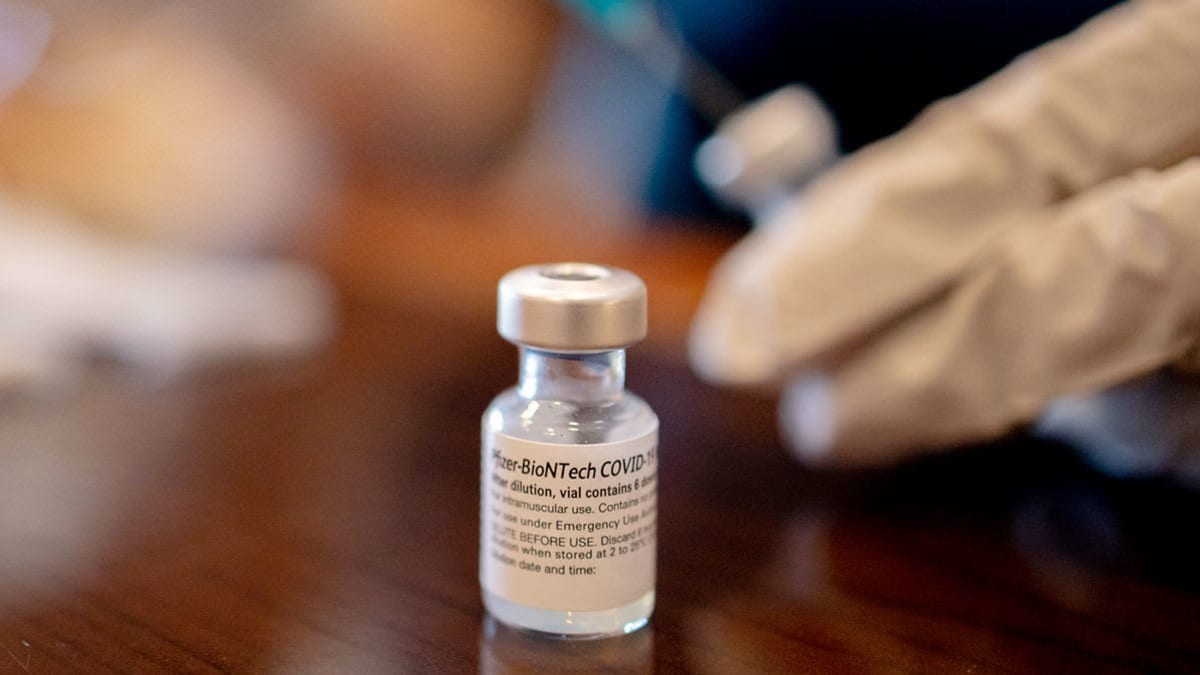
At the end of August, the FDA authorized booster shots with new formulas made by manufacturers Moderna and Pfizer-BioNTech, which replaced previous boosters for eligible populations. As part of that authorization, the agency said that anyone 12 or older who was fully vaccinated would be able to get the new updated boosters—referred to as bivalent boosters because they target both the original strain and two omicron subvariants, BA.4 and BA.5—as long as it had been two months since their last vaccine dose or booster shot. On September 1, the CDC recommended these same populations get the new boosters.
A little over a month later, public health officials expanded their recommendations to include younger populations as well. On October 12, the FDA authorized Moderna’s bivalent booster for kids ages 6 to 17, and Pfizer-BioNTech’s bivalent booster for kids ages 5 to 11. CDC director Rochelle Walensky recommended kids get access to bivalent boosters on the same day.
“Since children have gone back to school in person and people are resuming pre-pandemic behaviors and activities, there is the potential for increased risk of exposure to the virus that causes COVID-19,” Peter Marks, MD, PhD, director of the FDA’s Center for Biologics Evaluation and Research, said in a statement. "We encourage parents to consider primary vaccination for children and follow up with an updated booster dose when eligible.”
Who Is Eligible for a Booster Shot?
Now that the CDC has signed off on the updated boosters, anyone 5 or older who received their last booster shot or last required shot from the initial vaccination series at least two months prior can get one of the updated, bivalent boosters. Many people who got their second booster in the spring will be eligible for a third booster shot. As of Oct. 6, 2022, about 110.6 million people in the U.S. had received booster shots.
The updated Moderna boosters are authorized for people 6 and older. The updated Pfizer-BioNTech boosters are authorized for people 5 and older. No boosters are currently authorized for kids under 5.
Because the immune systems of many immunocompromised people don’t generate sufficient protection after the first two vaccine doses, researchers determined that a third dose—not technically a booster—is beneficial for many of them. This applies to those who are on immunosuppressant drugs after an organ transplant, as well as people who have a similar level of immune system impairment. People 12 and older who are moderately or severely immunocompromised and got an mRNA vaccine (Moderna or Pfizer) are eligible for their third vaccine dose four weeks after their second shot and a bivalent booster shot two months after that (for a total of four shots). Kids ages 5 to 11 follow a similar schedule, but wait three months for their fourth shot.
The first booster recommendation for immunocompromised people who received the single-shot J&J vaccine is the same as for everyone else who got a J&J shot—two months after the initial dose.
People who have been vaccinated with Novavax, which was authorized in July, can get a bivalent booster two months after their second shot.
What’s the Evidence That People Need Boosters?
While currently available vaccines—especially the mRNA vaccines made by Pfizer-BioNTech and Moderna—are highly effective, data shows that the protection they provide wanes over time. Boosters have been shown to restore that protection, and research indicates that a booster is particularly important for raising protection against the omicron variant.
In data that Pfizer and BioNTech submitted to the FDA when getting the first boosters authorized, the companies cited a preliminary study by the healthcare company Kaiser Permanente, which found that the vaccine’s efficacy against infections with the delta variant declined from 93 percent a month after initial vaccination to 53 percent four or more months after vaccination. Efficacy against hospitalization remained at 93 percent. Evidence presented by Pfizer indicated particular concerns about immunity waning for older people.
On Sept. 15, 2021, Moderna released data showing that people who were immunized with its vaccine between December 2020 and March 2021 were about 36 percent less likely to develop a breakthrough infection than those who were immunized between July and October 2020. The company said this apparent decline in protection supported the use of a booster dose. But it also said the vaccine was still about 95 percent effective at preventing hospitalization with COVID-19.
In its submission to the FDA requesting authorization for a booster dose, Johnson & Johnson said that while its vaccine remained highly effective against the most severe cases of COVID-19 (which resulted in hospitalization or death), its efficacy against moderate to severe COVID-19—which was lower than the mRNA vaccines from the start—had fallen over time, driven by reduced protection against variants of the coronavirus. During the FDA advisory committee meeting discussing J&J boosters, FDA and CDC experts stressed that the lower level of protection for people who had received only one J&J shot made a booster particularly important for this group.
Omicron significantly changed the booster calculus. According to one study published by the CDC, vaccines remained 76 percent effective against hospitalization more than six months after a second dose while delta was the predominant variant. Once omicron became the predominant variant, vaccine efficacy against hospitalization six months after a second dose fell to 57 percent. But two weeks after a booster dose, vaccine protection against hospitalization rose back to 90 percent.
In Pfizer and BioNTech’s request to authorize a fourth shot, the companies said that data from Kaiser Permanente Southern California showed that the protection an initial booster provided against infection and severe disease caused by omicron waned after three to six months.
For those who received their first booster months ago, the new updated boosters could shore up protection that has waned.
Boosters may be especially important for kids ages 5 to 11 because for this group the protection against infection with the omicron variant provided by two initial very small vaccine doses has been lower. “Since authorizing the vaccine for children down to 5 years of age in October 2021, emerging data suggest that vaccine effectiveness against COVID-19 wanes after the second dose of the vaccine in all authorized populations,” the FDA’s Marks said in a statement. “The FDA has determined that the known and potential benefits of a single booster dose of the Pfizer-BioNTech COVID-19 Vaccine for children 5 through 11 years of age at least five months after completing a primary series outweigh its known and potential risks and that a booster dose can help provide continued protection against COVID-19 in this and older age groups.”
Do Boosters Improve Immunity?
Yes. Data published by the CDC and peer-reviewed research published in medical journals show that boosters significantly improve immunity, including against the delta and omicron variants.
According to a study published Oct. 7, 2021, in The New England Journal of Medicine, a booster shot for people in Israel who were 60 and older and fully vaccinated at least five months earlier significantly reduced the risk for any breakthrough infection or for severe disease. Another NEJM study from Israel, published December 23, found that people who received a booster dose were approximately 90 percent less likely to die from COVID-19 than vaccinated people who had not received a booster. (Unvaccinated people are still far more likely to die from COVID-19 than people who have received two doses of an mRNA vaccine.)
CDC research indicates that boosters significantly lower the risk for hospitalization due to the delta or omicron variant. And a study published by CDC researchers in the journal JAMA shows that even though omicron is able to evade some of the protection against infection provided by vaccines, people who have received a booster are 66 percent less likely to test positive for omicron than people who received just two vaccine doses.
During an April 6 FDA advisory panel meeting discussing booster shots, the CDC presented data showing that while booster doses do indeed help prevent infection, their efficacy was highest against more severe cases and death. “The pattern here shows the clear benefit of a third dose during omicron,” said Lt. Cmdr. Ruth Link-Gelles, PhD, a CDC epidemiologist.
Still, research has increasingly shown that booster protection also wanes over time. According to a study released by the CDC on February 11, two months after a booster vaccine efficacy against an emergency room or urgent care visit was 87 percent, and efficacy against hospitalization at that point was 91 percent. Four months after the booster, efficacy against an ER or urgent care visit fell to 66 percent, and efficacy against hospitalization fell to 78 percent.
Pfizer and BioNTech said that in people 60 and older, Israeli data shows that a second booster dose raises antibody levels to the peak seen with the initial booster. Rates of infection and rates of severe illness are significantly lower among those who receive a second booster, the companies say.
While protection against any infection starts to fall about a month after the fourth dose, protection against severe disease and death lasts at least six weeks—and could last longer, according to an April 6 study in The New England Journal of Medicine.
In the FDA’s authorization for a second booster dose, the agency said data showed that the second booster dose raised antibody levels against both delta and omicron variants of the coronavirus.
There is as yet no real-world data showing how well the updated bivalent boosters protect against infection. But trial data shows that similar bivalent booster shots based on the original coronavirus strain and the BA.1 omicron subvariant did a better job raising immune system protection than boosters just based on the original coronavirus strain. These newly updated bivalent boosters are expected to perform even better against current variants, said the FDA’s Marks.
Are There Additional Risks From a Booster Shot?
The data presented during FDA and CDC meetings on boosters showed that side effects were similar to those after the second dose of an mRNA vaccine. And data shared by Pfizer and Moderna suggests that the same is true with the bivalent boosters.
So far, data evaluated by the FDA indicates that the benefits of a booster dose outweigh the risk of myocarditis (heart inflammation), a rare complication some people experience after a dose of an mRNA vaccine that has generally resolved quickly. Rates of myocarditis after a booster are much lower than after a second vaccine dose, according to a CDC study released March 1.
In kids ages 5 to 11, commonly reported side effects after a booster dose are similar to those effects seen after an initial or a second vaccine dose, including pain and redness at the injection site, fatigue, muscle or joint pain, and fever.
The FDA said no new risks were identified with a second booster dose based on several data sources, including an analysis of approximately 700,000 second booster doses given to people 18 and older in Israel. When authorizing boosters for younger populations, the FDA said people may experience side effects similar to those found with initial vaccines.
Should You Get the Same Shot You Got the First Time?
That’s up to you. “Eligible individuals may choose which vaccine they receive as a booster dose,” the CDC statement said. “Some people may have a preference for the vaccine type that they originally received, and others may prefer to get a different booster.”
A study conducted by the National Institutes of Health indicates that a Moderna or Pfizer booster may raise antibody levels for J&J recipients far more than a J&J booster. This research is still preliminary; more is underway on which boosters might yield the strongest protection for recipients of J&J, Moderna, and Pfizer vaccines.
Keep in mind that Moderna’s booster shot is a different dose from the first shots—50 micrograms instead of 100. So if you’re getting a Moderna booster, you’ll want to make it clear to the provider that you don’t want one of the initial shots. Pfizer’s and Johnson & Johnson’s doses are unchanged for booster shots.
While authorizing the updated boosters, the FDA revoked the authorization for the original monovalent Moderna or Pfizer-BioNTech boosters for people 12 and older, making bivalent boosters the only mRNA option.
Where Can You Get a Booster Shot?
They’re being given at the same sites where coronavirus vaccines are available, including hospitals, pharmacies, doctors’ offices, and clinics. You don’t have to get a booster where you received your initial vaccination, but remember to take your vaccine card with you. Check with your state health department, or search Vaccines.gov to find a location near you.
Will We Need Boosters Forever?
Down the road it’s possible that we may need a regular booster against the coronavirus as we do against the flu, says Joshua Barocas, MD, an associate professor at the University of Colorado School of Medicine who specializes in infectious disease.
But whether that’s the case depends on how well we control the ongoing pandemic, says Anna Durbin, MD, director of the Center for Immunization Research and a professor in the department of international health at the Johns Hopkins Bloomberg School of Public Health. The best way to ensure that we don’t need them soon or regularly is to stop the disease from spreading, and the best way to do that is to vaccinate the unvaccinated, both in the U.S. and around the world. The more unvaccinated people there are, the more chances there are for new variants to emerge.




