By the time Jeanne Rowe, M.D., became chief medical officer of Shore Medical Center in 2012, the small community hospital near Atlantic City, N.J., faced an alarming situation: Its intensive care units had reported 8 infections among its patients in the previous 12 months.
The infections were all traced back to central lines, the intravenous tubes used to supply medication, nutrients, and fluids to patients who need them most. But when not handled properly, central lines can also become host to bacteria, pumping germs straight into the bloodstream of the hospital's most vulnerable patients.
Once there, the bacteria—including "superbug" strains such as MRSA that aren't easily managed with antibiotics—can spread to the heart and other organs.
With that cluster of cases, Shore Medical Center then rated as one of the worst in the country at preventing the infection, according to Consumer Reports' hospital ratings—a situation Rowe was well aware of.
And if the poor infection record wasn't fixed, it could cost the hospital more than its reputation. President Barack Obama had recently signed the Affordable Care Act, and among its provisions was one that lowered Medicare payments to hospitals that had too many of these infections.
Rowe, a physician who specializes in internal medicine, had a proven record for improving patient safety at several hospitals where she had worked in the Midwest. "We knew we had to do something about it," she says now.
Costly, Deadly—and Avoidable
About 650,000 people developed infections after being admitted to U.S. hospitals in 2011, and 75,000 died, based on the most recent data from the Centers for Disease Control and Prevention. That would make hospital-acquired infections the nation's eighth leading cause of death, just behind diabetes and just ahead of flu and pneumonia.
Central-line infections account for roughly 5 percent of all hospital-acquired infections, striking more than 27,000 people in 2015, research shows. And they're a particularly important subset, says Arjun Srinivasan, M.D., associate director for Healthcare Associated Infection Prevention Programs at the CDC.
Read Consumer Reports' position on what needs to happen to keep patients safe.
For one, they are deadly—proving fatal in up to a quarter of cases, in part because people with the IVs are often already frail. They're costly, too, averaging $46,000 to treat, more than other hospital-acquired infections, according to a 2013 study in the Journal of the American Medical Association.
And they're almost entirely preventable.
As far back as 2001, Peter Pronovost, M.D., now senior vice president for patient safety and quality at Johns Hopkins Medicine in Baltimore, developed a safety checklist similar to one used by pilots prior to takeoff. He showed that when ICU staff adhered to the protocol, central-line infections could be sharply reduced, even eliminated.
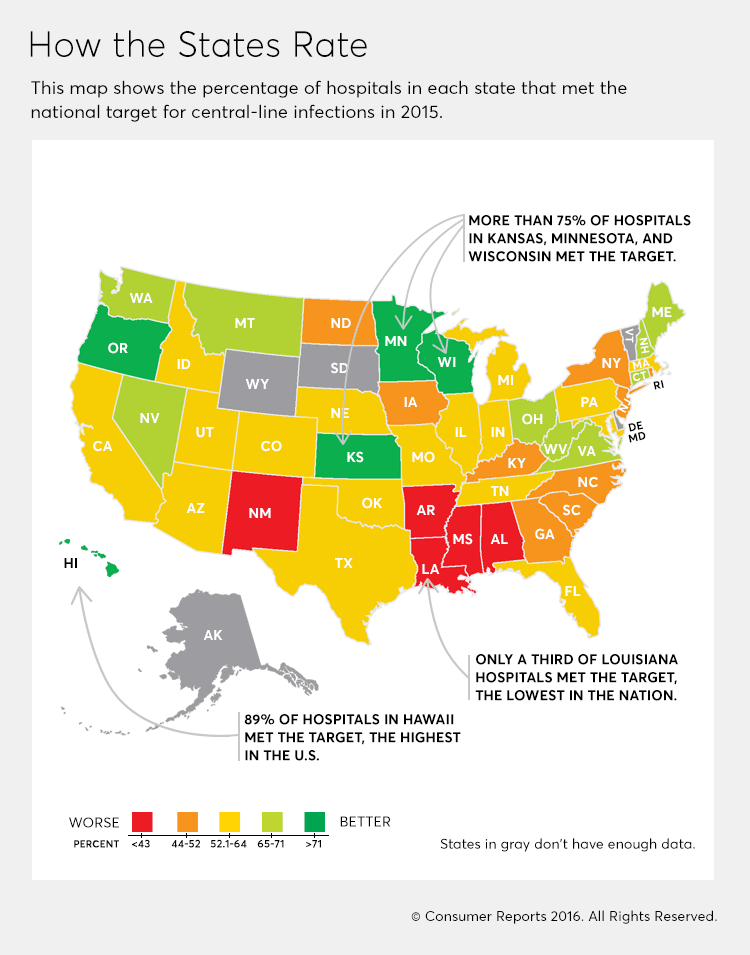
Defeating a Deadly Infection
When she arrived at Shore Medical Center, Rowe doubled down on making Pronovost's checklist a priority.
Posters of men and women in Uncle Sam pose—right arm out, finger pointed—with the words "I Want You to Wash Your Hands" were hung all around the hospital. Extra soap and alcohol gel dispensers were placed in and around patient rooms. Nurses began swabbing every patient's skin with chlorhexidine, a powerful antiseptic, before inserting central lines, then again when the dressing needed changing.
Fewer central lines mean fewer chances for hospital-acquired infections, so physicians reviewed every day which patients really needed the IVs. A secret team was deputized to roam the hospital and report staff who didn't wash their hands before seeing patients. "People behave much better when they think someone is watching," says Valerie DeJoseph, director of quality at the hospital.
Soon, the extra effort paid off. In Consumer Reports' most recent ratings of about 2,000 hospitals nationwide, Shore Medical Center earned top marks, going 21 months without reporting a single central-line infection.

Still Too Many Infections
Pronovost's protocols, combined with the threat of reduced federal funding and more public accountability, seem to have helped not just Shore Medical Center but many hospitals.
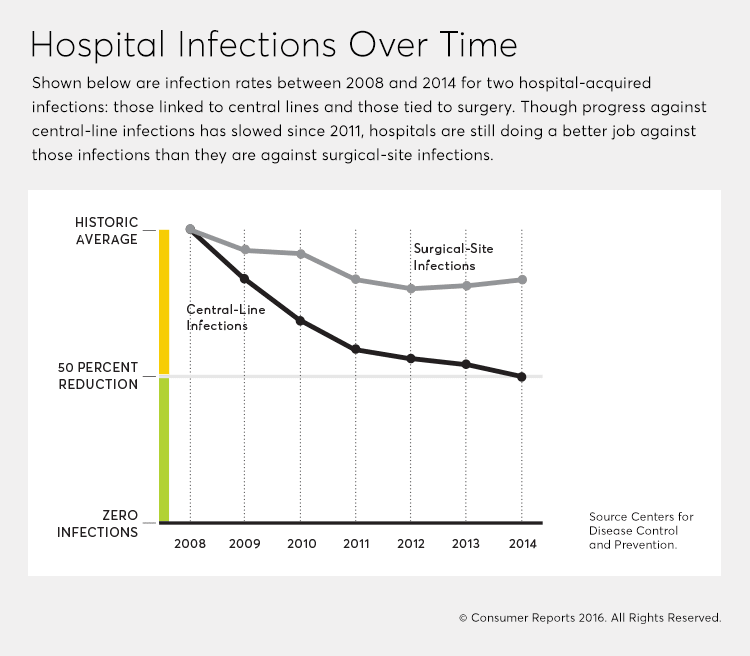
Though other hospital infections have stayed steady or declined only slightly in recent years, those linked to central lines were cut in half between 2008 and 2014, according to the CDC. "It's one of the nation's greatest patient-safety success stories ever," says Srinivasan.
Consumer Reports' analysis found improvement all around the country, in large urban hospitals such as Ochsner Medical Center in New Orleans and Johns Hopkins Bayview Medical Center in Baltimore, as well as smaller suburban or rural ones like Wuesthoff Medical Center in Rockledge, Fla., and Mercy Medical Center in Merced, Calif.
And yet the problem isn't solved, says Doris Peter, Ph.D., director of Consumer Reports' Health Ratings Center. "Hospitals are moving in the right direction, but progress is slowing and too many hospitals have not adequately addressed the problem of hospital-acquired infections over the past five years."
That's true even among the nation's prominent teaching hospitals, such as Dartmouth-Hitchcock Medical Center in Lebanon, N.H., and Ronald Reagan UCLA Medical Center in Los Angeles, both of which appear on our list of low-scoring teaching hospitals (see below). "That's counterintuitive," Peter says. "They are supposed to be places that represent the best in our healthcare system."
Administrators at these hospitals say they are responding. "We identified a problem with our infection rate two years ago and immediately took corrective action," says George Blike, M.D., chief quality and safety officer at Dartmouth. As a result, he says, the hospital's most recent data—not yet published by the government and thus not reflected in our ratings—show that infection rates are dropping.
And though hospital administrators say they use versions of the Pronovost checklist, they also say their hospitals face special challenges. For example, Ronald Reagan UCLA says its high infection rates were due in part to "the complexity of the medical cases and the severity of illness that we treat."
But the CDC actually does try to adjust for those factors. In addition, Consumer Reports' analysis found no clear evidence that hospitals with more Medicaid patients—an indication that they treat sicker or underserved populations—perform worse than hospitals with fewer Medicaid patients.
In addition, there are examples around the country of hospitals that serve similar underserved populations but perform very differently against these infections. For example, Maimonides Medical Center in Brooklyn, N.Y., appears on our list of teaching hospitals with few central-line infections, while nearby SUNY Downstate Medical Center University Hospital has higher-than-expected rates of those infections.
SUNY Downstate is responding by trying to encourage a "culture of safety" among all team members, says Michael Augenbraun, M.D., director, division of infectious diseases at SUNY Downstate Medical Center.

The Path to Zero
Central-line infections were once seen as inevitable when dealing with patients in intensive-care units. "We thought we could maybe cut them by 10 percent," says Srinivasan, at the CDC.
But in 2004, Pronovost, at Johns Hopkins, put his checklist to the test at more than 100 Michigan ICUs. "Within three months, rates were cut in half," he says, and by 18 months it was down by almost 70 percent. "If hospitals are meticulous about following the checklist, most infections can be avoided," he says.
But that requires buy-in from everyone—from senior administrators and physicians to cleaning staff and nurses.
Maureen Jewell, R.N., director of quality management and performance improvement at Saint Francis Hospital in Wilmington, Del., says it was important to make hospital-acquired infections everyone's problem to solve.
"We spent much of our time empowering nurses to speak up if hospital staff weren't following the checklist carefully," she recalls. "We had to make it clear that when it came to these infections, the physicians weren't calling the shots—they were." Like Shore Medical Center in New Jersey, Saint Francis Hospital improved from one of the lowest-performing hospitals in 2011 to one of the highest-rated ones.
Even some large hospitals in urban areas have improved. One that stands out: Mount Sinai St. Luke's-Roosevelt Hospital, in New York City. On the day we visited in October 2016, the whiteboard outside one of its ICUs proclaimed it had gone 969 days without a single central-line infection.
To keep that streak alive, the hospital staff is constantly reassessing how it's doing. For example, a monthly staff meeting recently revealed that some nurses weren't using a new, more effective antiseptic dressing because it wasn't included in the prepackaged kits used to insert a central line, says Emilia Mia Sordillo, M.D., the physician in charge of infection prevention at the hospital. By the end of the week, "all the kits had the right antiseptic dressing," she says.
Rowe, the medical director at Shore Medical Center, says preventing the infections is not costly or all that complicated. It just takes training and patience and commitment to doing the little things right "every single day, every single patient."
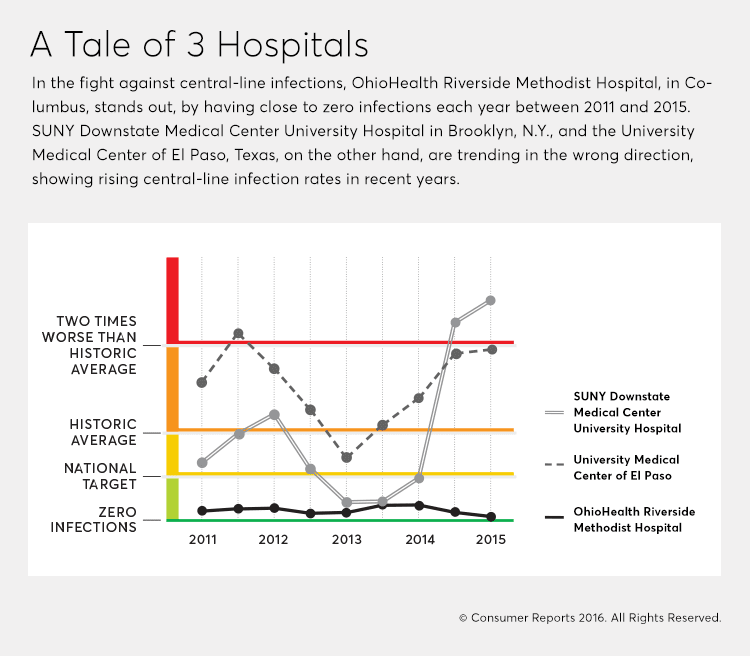
Preventing Central-Line Infections
The lists below show the highest- and lowest-performing U.S. teaching hospitals at preventing central-line infections in intensive care units from Jan. 1, 2011,to Dec. 31, 2015, the most recent federal data that's publicly available. Hospitals are listed alphabetically. Read more on these hospitals, including their ratings, plus information on how we rate hospitals on central-line infections (PDF).
Lowest-Scoring Teaching Hospitals
Highest-Scoring Teaching Hospitals
Keeping Patients Safe: What Needs to Happen
Consumer Reports first focused on hospital infections in 2003, when we urged states to pass laws requiring that hospitals publicly report those events. Once hospitals began doing that, we started rating them on infections, hoping "it would nudge hospitals toward solutions," says Lisa McGiffert, director of Consumer Reports' Safe Patient Project. That has helped, but more needs to be done.
CR believes that the federal government should require hospitals to:
• Immediately report infection outbreaks or infection-control breaches to patients, healthcare providers, state and federal agencies, and the public.
• Undergo inspections that check not only for infections but also whether they have instituted comprehensive infection-control programs involving everyone from the cleaning staff to the CEO.
• Provide a system for patients to report when infections occur, to improve tracking of those events.
Did you or a loved one develop an infection while in the hospital? Share your story.
Editor's Note: This article also appeared in the January 2017 issue of Consumer Reports magazine.