How to Choose and Use a CPAP Machine for Sleep Apnea
Struggling with this sometimes challenging therapy? Our CPAP guide can ease your way and help you get a better night's rest.
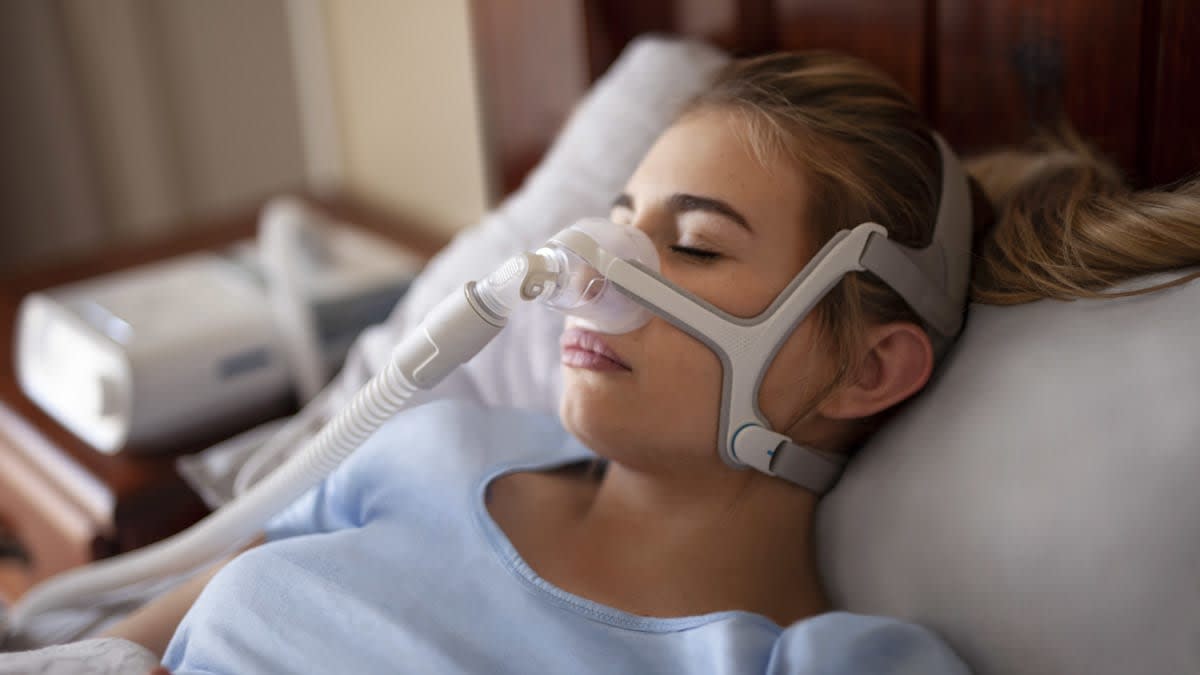
If you’ve received a diagnosis of obstructive sleep apnea (OSA)—which causes numerous brief pauses in breathing as you sleep—your doctor has probably recommended continuous positive airway pressure (CPAP) as a treatment.
With CPAP, the mainstay treatment for the disorder, you typically wear a masklike apparatus that’s connected to a pump. The pump pushes air into your airway, holding it open while you sleep.
How CPAP Machines Work
There are currently approximately 5.9 million OSA diagnoses among U.S. adults, according to the American Academy of Sleep Medicine. In those with the disorder, neck and throat muscles relax during sleep, causing the soft tissue at the back of the throat to collapse and block air from reaching the airway. That causes a series of partial or complete pauses in breathing, sometimes hundreds of them each night.
CPAP—which sends enough air into the upper airway to prop it open—has been the cornerstone of therapy for moderate to severe OSA since the 1980s.
The prescription treatment has been shown to improve sleep quality, reduce daytime sleepiness, help normalize blood pressure, and ease other related health risks.
For instance, a study published in 2018 in the Journal of the American Heart Association of more than 40,000 Danish adults with sleep apnea found that those who skipped CPAP had a 38 percent higher risk of heart failure than those who used it.
Not only can CPAP be effective, but the machines are now easier to tolerate—quieter and less clunky than older devices.
Many newer CPAPs allow you to start the night at a lower air pressure setting—and have that pressure rise gradually after you fall asleep. This can reduce the jarring feeling of air being forced into your nose or mouth.
Some CPAP units even adjust automatically to patterns in your breathing, increasing or decreasing air pressure throughout the night as needed.
How to Choose a CPAP Machine
Finding a CPAP mask that is comfortable enough to allow you to slumber is essential. (You’ll also consider factors like the severity of your OSA and the air pressure setting your doctor has recommended to keep your airways open during sleep.)
But this can take time. Even with the advances above, using a CPAP machine can feel clumsy and awkward, according to Steven Feinsilver, MD, a sleep medicine specialist at Lenox Hill Hospital in New York City. "Most people do not end up with the first device they try. Some people may try two or three before finding the right fit," he says.
That was the case for Hb Alumisin, 33, of New York City, who tried two masks before settling on a third option—nasal pillows (see below)—for his mild sleep apnea.
"I found the masks heavy and hard to sleep with, but the pillows are comfortable and less obtrusive," he says.
At your fitting (which may be done at home or at a sleep center), "try masks on with the doctor-recommended air pressure settings you’ll be using to see what it really feels like when the machine is on," Dasgupta advises.
And make sure any device you’re considering fits snugly enough to form a seal where it’s meant to, Dasgupta says, but not so tightly that it leaves marks on your face.
There are three main types of CPAP masks available:
Nasal pillows. The "pillows" are small plastic plugs that rest directly below the nostrils and direct airflow to your nasal passages. Nasal pillows are the smallest, most lightweight option and require minimal contact with the user’s face.
Pillows may work best for people who require a low to moderate air pressure setting and may be a good option for people with a lot of facial hair or who feel claustrophobic wearing a larger mask, according to the American Academy of Sleep Technologists (AAST).
But they may cause nasal irritation and discomfort, especially at higher-pressure settings, because air is being forced directly into the nostrils. Some users report nosebleeds or nasal dryness. Mouth breathers may not get as much benefit from this type of mask because it applies pressurized air only to the nasal passages.
Nasal mask. This mask will cover your face from the bridge of the nose to the top of your upper lip, creating a seal over your nose but not your mouth. The AAST recommends nasal masks for people who want a more natural-feeling airflow than they’d get with nasal pillows.
"Some people prefer the mask to the pillows because the air is not as concentrated. Spread out over a larger surface area, it may have a more comfortable feel," says Edwin Valladares, a CPAP user who works as a sleep technician and manager of the Sleep Disorders Center at Keck Medicine of USC.
The nasal mask may not be best for people who are mouth breathers or those who have trouble breathing through their nose because of allergies, sinus blockages, or medical conditions such as deviated septum. Some people find that the mask causes irritation or discomfort on the bridge of the nose.
Full face mask. This type of mask covers both the nose and mouth, forming a seal over both airways. A full face mask may be a good option for people with allergies or medical issues that make it difficult for them to breathe through their nose during sleep. It may also work for those who need a higher-pressure setting but find this more comfortable than a nasal mask, the AAST says. But the bulkiness may be a drawback for some folks.
Tips for Using a CPAP Machine
It may take two to three weeks to get comfortable sleeping with CPAP and four to six weeks before you really begin to see a benefit, according to James Rowley, MD, medical director of the Detroit Receiving Hospital Sleep Disorders Center.
A gradual introduction to CPAP works best for many people, Feinsilver says. Start by using your CPAP for 20 to 30 minutes before bed. "Put the mask on, turn the machine on, and watch TV or read a book," he says. After a few days, try sleeping with the device. "If you don’t fall asleep within an hour, take it off and try again the next day," Feinsilver says.
If you find that the mask that felt right during your fitting is uncomfortable after a few nights, or that it’s difficult to adjust, contact your sleep medicine doctor or the medical equipment provider. You may need advice on adjusting or a different style of mask.
And if after two to three weeks of giving it a good try, you feel that CPAP just isn’t working for you, "talk with your sleep physician about what else you can do, but don’t just quit," Rowley says.
For some people, it may take additional time to adjust. David Levey, for instance, estimates that he spent two to three months to feel fully comfortable with his CPAP—and to switch from a side sleeping position to a back position to keep his device from slipping out of place.
"Getting used to sleeping on my back was the hardest part about adjusting to CPAP, but once I did I woke up feeling so much more refreshed," he says.
Handling Common Side Effects of CPAP Machines
Side effects from wearing a CPAP can often cause discomfort. Here’s how to handle common CPAP-related complaints:
Dry mouth. An uncomfortably dry mouth can occur when a full mask fails to form a tight seal over your face or with a nasal mask or nasal pillows if you’re mouth-breathing, says Rowley.
What to do: If you wear a full mask, have your sleep medicine specialist or sleep technician check the fit. For mouth-breathing, ask whether a chin strap can be added to your nasal mask or nasal pillow devices to hold your mouth shut during sleep.
Nasal congestion. This can be the result of air being directed into your nose.
What to do: Most newer CPAP machines come with a built-in humidifier—you can adjust the level of humidification so that it might ease nasal congestion. If that doesn’t help, talk to your doctor. "Most CPAP-related nasal congestion can be treated with an antihistamine or nasal steroid spray," Rowley explains.
Rash. Some CPAP users report redness, itching, or rash where the mask touches the skin. According to the AAST, an allergic reaction to a CPAP mask is rare and such skin problems are almost always related to improper mask hygiene.
What to do: "Wash the entire mask and humidifier chamber with soap and water at least once a week," Rowley says. (Get more CPAP care tips here.) And while some researchers have theorized that CPAP might increase the risk of respiratory infections such as pneumonia, studies so far have failed to find a link.
Sleep Apnea Treatment Alternatives
Non-CPAP treatment options are also available, including mouth guards, called mandibular advancement devices, that help to keep your airway open, and surgically implanted devices that deliver electrical impulses to the nerve that controls the upper airway muscles.
If you’re overweight, shedding some pounds can help reduce sleep apnea severity, too.
And remember this: "Not only will addressing your sleep apnea help you sleep better, but you might live longer," Feinsilver says.




