Sign In

Tens of millions of Americans live with medical devices implanted in their bodies—artificial joints, heart defibrillators, surgical mesh. And it's a safe bet that most of them assume that someone, somewhere, tested the devices for safety and effectiveness.
But that is rarely the case. For most implants and other high-risk devices brought to market, manufacturers do nothing more than file some paperwork and pay the Food and Drug Administration a user fee of roughly $4,000 to start selling a product that can rack up many millions of dollars in revenue. Often, the only safety "testing" that occurs is in the bodies of unsuspecting patients—including two of the three people whose stories are told in this report.
As for the smaller number of high-risk products for which advance safety studies are required, government rules allow them to be sold based on studies that are smaller and less rigorous than those required for prescription drugs.
"Standards for devices exist, they just don't make sense," says Diana Zuckerman, Ph.D., a vocal critic of the current system and president of the National Research Center for Women & Families, a nonprofit advocacy organization.
In 2011, a panel from the prestigious Institute of Medicine said the FDA should overhaul its device regulatory system because it fails to ensure patient safety before and after products go on the market. Instead, Congress is now debating a new law that would keep the present system virtually intact and ratify an agreement between the FDA and industry to get devices on the market even faster.
The FDA believes "the program has served American patients well," says Jeffrey Shuren, M.D., director of the agency's Center for Devices and Radiological Health. "As a responsible guardian of public health, the FDA believes it's a challenge to eliminate a program without having a better alternative."
But an investigation by Consumer Reports, which included interviews with doctors and patients and an analysis of medical research and a device-safety database maintained by the FDA, shows the following areas of concern:
Below are stories from three people, injured by three very different devices, that highlight the dangers consumers face in the current marketplace.

In 2007, Janet Holt of Floresville, Texas, felt swelling in her pelvic area. She went to her gynecologist, who told her that her bladder and uterus had prolapsed—dropped out of their normal position within her pelvis. The doctor recommended a hysterectomy and bladder lift.
"He talked about building a little bird's nest to hold my bladder up," Holt recalls. "He said I'd be back at work in two weeks." She has yet to return to work full-time on the cattle ranch and small chain of restaurants she runs with her husband.
The "bird's nest" turned out to be a sheet of synthetic mesh that was implanted by instruments inserted through the walls of her vagina. In the weeks and months after surgery, she says, "I was in such pain I couldn't sit, I couldn't stand, and I could hardly walk." Over time, the mesh shrank and shifted, eventually working its way back out of the vaginal wall, an experience Holt likens to "open cigarette burns with each step you take. It's complete torture."
Today, after eight surgeries to adjust and remove the mesh, Holt, who is suing the device manufacturer, says she has been left with painful nerve damage in one leg. "I'm 54 years old and it has totally ruined my life," she says.
Holt is one of hundreds of thousands of women implanted with transvaginal mesh for prolapse repair and bladder support since the first such products came on the market in the early 2000s. Manufacturers marketed the mesh packaged in a "kit" with tools for insertion and marketed them to doctors as an easier way to do a surgery that had traditionally required special additional training.
"The companies were saying, ‘The salesman will show you how to do it,' " said Lewis Wall, M.D., professor of obstetrics and gynecology at Washington University in St. Louis. Despite thousands of reports of adverse events, repeated alarms by women's-health and consumer-health advocates, and multiple lawsuits, these products are still being sold—and are still classified as "moderate risk" devices.
In an August 2011 petition asking the FDA to take transvaginal mesh off the market, the consumer advocacy group Public Citizen called it "a ‘poster-child' example of the fundamental failure ... to protect the public's health and welfare."
How did it happen? The mesh manufacturers took advantage of a loophole in the law that allowed them to grandfather their products onto the market without any advance safety testing.
Here's how it works: Before 1976, a manufacturer could sell virtually any medical device at will. That year, a new law for the first time classified medical devices into three risk categories, with clinical data required only for devices in the highest-risk category, Class III.
The FDA has yet to fully enforce even that minimal testing requirement. The agency routinely clears new devices in all three risk classes without clinical testing as long as manufacturers can show they are "substantially equivalent" to a device that has already been on the market.
And that's exactly what the makers of transvaginal mesh did. The mesh kits were cleared based on their "substantial equivalence" to an earlier mesh used to repair abdominal hernias that was sold as long ago as the 1950s, even though the kits were designed to be used in a different part of the body and inserted laparoscopically, not through open surgery.
"You're putting a foreign object into the pelvis through a contaminated space, so there's a very high potential risk of infection," Wall says. "But there weren't any clinical trials done with these products before they hit the market."
"The paradox is that companies go to the FDA and claim that a device is ‘substantially equivalent,' but when they market it, they claim it's ‘new and better,' " says Rita Redberg, M.D., a professor of medicine at the University of California, San Francisco, and editor of the Archives of Internal Medicine. The clearance process costs manufacturers next to nothing; they pay the FDA a user fee of $4,049.
It was only in January 2012, about 10 years after the first kits hit the market, that the FDA took action. It ordered 33 companies to conduct the first-ever post-market safety studies of the products. The agency is thinking of reclassifying those mesh kits to the highest-risk Class III.
But Shuren, at the FDA, notes that with the government's rule-making process, "from the time the FDA decides to upclassify a device to the time it can actually do it can take years."

In 2009, after many unsuccessful diets, Lisa Wilson, then 46, a pharmacy technician from Seattle, received the Lap-Band adjustable gastric band.
The implanted band constricts the size of the stomach to make it difficult to eat large quantities of food. In fact, the opening left to Wilson's stomach was so small that she had difficulty eating even small amounts of food. It also caused her to throw up almost every day.
But she stuck with it, losing 70 pounds, until a routine endoscopy in December 2010 revealed that the band had cut into her stomach lining and would have to be removed immediately. She developed a post-surgical infection that resulted in a partially collapsed lung and an eight-day hospital stay. Wilson says she has regained half of the weight she lost.
More than 650,000 Lap-Bands have been sold worldwide, according to the 2010 annual report from its manufacturer, Allergan. It's among the minority of devices so novel that manufacturers can't find an older product for grandfathering.
Those products usually have to undergo advance testing for safety and effectiveness to get the FDA's approval for marketing. But the tests aren't nearly as rigorous as those required for prescription drugs, even though, as Redberg notes, "if you have a problem with a drug, you can just stop taking it, but you can't do that for a device implanted in your body."
And the FDA charges device manufacturers only $220,050 to review a new device, compared with the $1.84 million it charges to review a new drug application.
If Lisa Wilson had seen the lone study on which the approval was based, she might not have been surprised by her problems. Of the 299 people in the study, 51 percent reported nausea, vomiting, or both, and 25 percent had their bands removed before the end of the three-year study because of complications or failure to lose enough weight.
"Imagine if a car had a recall rate that high," says John Santa, M.D., director of the Consumer Reports Health Ratings Center. "Consumers and regulators would be up in arms. But in the world of medical devices, these things often stay hidden."
The Lap-Band clinical trial was fairly typical of such pre-marketing studies. Redberg and colleagues looked at 123 studies done on high-risk cardiovascular devices that received FDA approval between 2000 and 2007. Only 27 percent met the gold standard of being randomized clinical trials, according to the report, published in December 2009 in the Journal of the American Medical Association.

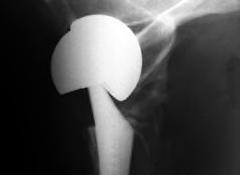
If any patient should have gone into a hip replacement fully informed, it was Stephen Tower, M.D., 55, an orthopedic surgeon from Anchorage, Alaska. Instead, he became the victim of another device that was grandfathered onto the market without clinical testing.
In this case, it was an artificial hip introduced in 2005 by DePuy, the orthopedic division of Johnson & Johnson. Called the ASR XL (shown at the top of this page), it was distinctive because both components—the ball at the top of the femur and the socket liner inside the pelvis—were made of chrome-cobalt metal.
The FDA cleared it without clinical testing based on "substantial equivalence" to earlier devices, though such metal-on-metal hips had long been on the agency's high-priority list for requiring advance clinical trials.
The all-metal hips were supposedly a great advance over hips with the traditional plastic socket liner, Tower recalls. "The main reason hips traditionally failed was because of plastic wear," he says. "The metal-on-metal hip was being promoted not only commercially but in the medical literature as being a solution for patients like me, who wanted to return to no-holds-barred physical activity."
By 2006, Tower's arthritic hip had forced him to give up practically all the outdoor pursuits he had moved to Alaska to enjoy. He had a DePuy ASR XL implanted in May of that year, and "within six weeks I did a double century bike race," he says. He was so enthusiastic that within 10 months he had put various models of metal-on-metal hips in six of his patients.
But by the time a year had passed, it became clear that something was wrong. His hip was "pretty much constantly painful" and the chromium and cobalt levels in his blood "were notably high," he says.Then he started noticing other problems, such as disturbed sleep, mood swings and anxiety, hearing loss, visual problems, and tinnitus.
Throughout that period, he says, he repeatedly questioned DePuy engineers, design surgeons, and sales representatives, "and they'd say, ‘Geez, Steve, we haven't heard of this.' "
Tower's symptoms became so severe at times that he was unable to work. Meanwhile, his research, some of which he has since published in medical journals, was uncovering evidence that metal debris from joint implants can cause what he describes as "profound poisoning."
After having the hip removed in 2009 and replaced with a new one made of ceramic and plastic, his symptoms have markedly improved.
In August of 2010, DePuy recalled all 93,000 ASR XL hips worldwide after it became clear that the device was failing far more often than average and producing serious injuries. While it's unclear how many people actually have had to have their artificial hip removed, an article in the British Medical Journal called it "one of the biggest disasters in orthopaedic history."
Although the hip was invented and manufactured by an American company, the recall occurred because as early as three years previously—even as DePuy's engineers were assuring Tower that the hip had no problems—regulators in Australia, England, and Wales were noticing serious problems.
They were able to do so because they have national joint registries—a list of every joint implanted—and the ability to track how patients fare with various models. There is no such national registry in the U.S., although Kaiser Permanente has a large private one.
The FDA has a voluntary system whereby doctors, manufacturers, and patients can report problems with medical devices. And though experts estimate that only a fraction of device problems ever get reported, from 2009 through 2011, the agency received 20,518 reports of injuries from metal-on-metal total hip replacements. Of those, 15,137 concerned the now recalled DePuy hip. Many of the remaining complaints concerned several other brands and models that are still on the market in the U.S.
The 2011 Institute of Medicine panel concluded that the FDA's ability to spot problems is so inadequate that it's "impossible to confidently draw broad conclusions about the safety and effectiveness of products that are on the market."
Consumers Union, the advocacy arm of Consumer Reports, agrees with the Institute of Medicine that the current system of medical-device regulation doesn't protect patients from harm. Consumers Union recommends that the FDA:
Have you had a problem? Tell us about it now. If you've had a problem with an implant or a medical device, please tell Consumer Reports about your experience. Your information is kept confidential (unless you indicate otherwise) and your story helps us monitor medical problems, research future articles, and push for reform.
To help, go to SafePatientProject.org and click on "Share Your Story" or click on "Act Now" to help us work for change.
Here are a few steps you can take to guard against the risks posed by dangerous medical devices.
Consider alternatives. Ask your doctor what will happen if you don't get the implant. Many women who received transvaginal mesh for prolapse repair, for example, probably never even needed surgery.
"Pelvic organ prolapse is almost never a life-threatening condition. It's a quality-of- life issue," explains Daniel S. Elliott, M.D., assistant professor of urology at the Mayo Clinic College of Medicine. "The overwhelming majority of women do not need to have surgery. If you're not bothered by it, then don't do anything. I think many patients weren't adequately informed about that."
You may also have non-mesh alternatives. Elliott says he and other well-trained pelvic surgeons routinely repair prolapses with techniques that don't require any mesh at all. On the other hand, people ill enough to need an implantable defibrillator for their heart may not have another choice.
Research the device. The Food and Drug Administration's website, FDA.gov, has a wealth of information about device safety warnings, complaints, and recalls, easily accessible by typing the name of the device into the site's search box. It's also worth searching Google. If the results include a lot of law firms looking for clients injured by the device, that's a sign to ask your doctor some hard questions.
For an optional device like a Lap-Band or breast implant, look around the Internet for patient forums. Though the information there isn't validated, you'll get a sense of whether patients are reporting trouble with the device.
Write down what you got. If your doctor doesn't give you information about the brand name, model, and serial number (if it exists) of your device, ask for it. If you learn of a warning or safety recall, from the FDA or elsewhere, you'll know whether yours is one of the problem models.
Stay alert—but don't panic. If you learn that there are problems with your device, contact your doctor and ask what warning signs to watch for. Also go to the FDA website to read up on official warnings and find out whether it's safe to keep the device in your body.
For example, if you have a metal-on-metal hip, call your doctor if you have pain or other unusual new symptoms, such as heart, vision, hearing, emotional, or neurological problems, because all of those might be signs of a reaction to the device. You might also want to get your blood tested for high cobalt levels, a sign that the hip is deteriorating.
But don't assume that all problematic devices have to be removed. For example, pelvic surgeons say they often get calls from worried women who have had mesh repairs. "If the mesh is not causing any problem, don't do anything because getting mesh out is very difficult and dangerous," Elliott says.
Cardiac devices dominate the list of reports to the Food and Drug Administration of deaths and injuries. Here are three devices that have had significant problems in recent years:
Implantable cardioverter-defibrillators. Since 2009, the FDA has received reports of close to 29,000 deaths or injuries from these devices, by far the most for any device type, according to our analysis of the FDA's database of adverse events. Implanted in more than a half-million Americans with serious heart disorders, the defibrillators detect abnormal rhythms and administer shocks to correct them.
The most troublesome aspect of the devices are the leads—wires that connect them to the heart. There have been two major recalls, in 2007 and 2011, of defective leads, the Medtronic Sprint Fidelis and the St. Jude Riata, after they had already been implanted in almost 350,000 patients. Patients with the device leads require close monitoring and face the prospect of having to have them surgically removed.
In congressional testimony in 2009, Boston cardiologist William Maisel, M.D., described what happened to a patient of his: "The simple act of removing his shirt over his head caused his … lead to fracture. [He] suffered a cardiac arrest in front of his wife." The patient survived but never fully recovered.
Vena cava filters. These devices are placed in the vessel that returns blood from the lower body to the heart to prevent pulmonary embolism, a life-threatening condition caused by blood clots breaking loose from the leg and traveling to the lungs. Some 200,000 people get such filters each year.
Many should be removed once the danger of clots has passed, but often aren't. In a November 2010 study in the Archives of Internal Medicine, Pennsylvania researchers found that pieces of the Bard Recovery filter had broken off and migrated elsewhere in the body in one of four study patients. One patient needed open-heart surgery.
"Remarkably," wrote cardiologist Rita Redberg, M.D., of the University of California, San Francisco, in an editorial accompanying the report, these filters "were considered Class II by the FDA—the same risk category of mercury thermometers—and received approval without any clinical data of safety and effectiveness."
"The devices were being used inconsistent with their FDA clearance," says Jeffrey Shuren, M.D., director of the agency's Center for Devices and Radiological Health. "We don't have authority to do something about that." If you've received the device, ask your doctor whether it has been removed.
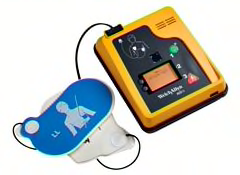
Automated external defibrillators. Found in airports and other public buildings, these devices are designed so that bystanders can operate them. AEDs automatically diagnose abnormal heart rhythms and deliver shocks to people in cardiac arrest.
The problem is, they don't always work. The industry has conducted about 90 recalls over the past several years, affecting hundreds of thousands of devices. Between 2009 and 2011, the FDA received reports of 72 injuries, 686 deaths, and 20,667 malfunctions connected with the devices. Arizona researchers found that in most cases the machines weren't able to diagnose the abnormal rhythms properly or failed to deliver the recommended shock.
The FDA is considering whether to downgrade AEDs from the highest-risk category to moderate-risk. recalled Defibrillators have been recalled 90 times in seven years.
A version of this article appeared in the May 2012 issue of Consumer Reports magazine with the headline "Dangerous Devices."
 Build & Buy Car Buying Service
Build & Buy Car Buying Service
Save thousands off MSRP with upfront dealer pricing information and a transparent car buying experience.
 Get Ratings on the go and compare
Get Ratings on the go and compare
while you shop