Health
Get expert reviews and ratings for health, fitness, and food products from Consumer Reports, and read the latest on drugs, hospital safety, and more.
Inside Our Test Labs
CR’s engineers test and rate thousands of products so that you can make great choices, based on data.
Exercise & fitness
Get the latest in-depth reviews, ratings, and buying advice for exercise & fitness products.
Food
Get the latest in-depth reviews, ratings, and buying advice for food products.
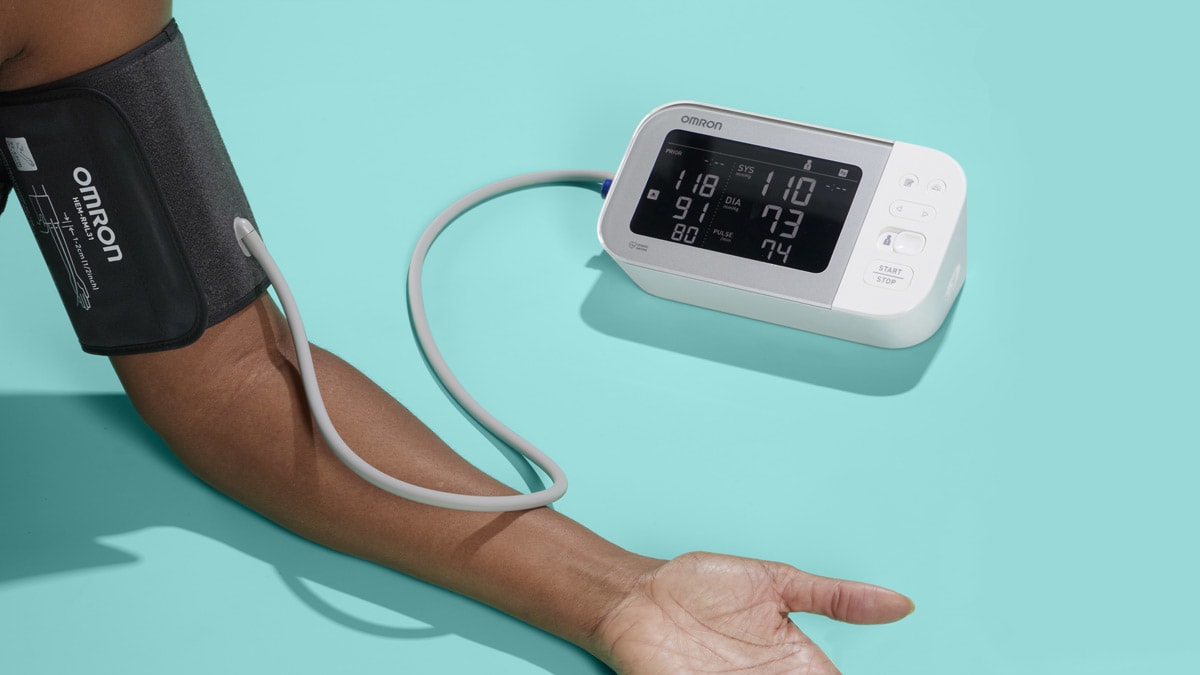
Home medical supplies
Get the latest in-depth reviews, ratings, and buying advice for home medical supplies.
Beauty & personal care
Get the latest in-depth reviews, ratings, and buying advice for beauty & personal care products.
Make an Impact
An independent, nonprofit member organization that works side by side with consumers for truth, transparency, and fairness in the marketplace.
Mission-Driven Nonprofit
Promoting truth, transparency, and fairness
Consumer-Centric
85+ years of advancing consumer interests
Independent
No advertising, sponsorships, or free samples for testing
Learn about free membership benefits & more