Sign In


Although some hospitals are doing an excellent job of preventing hospital-acquired infections, others are not, according to our recent analysis.
We focused on one of the most dreaded types of the approximately 1.7 million infections that occur each year in U.S. hospitals. They are bloodstream infections introduced through the large intravenous catheters that deliver medication, nutrition, and fluids to patients in intensive care. These so-called central-line infections account for about 15 percent of all hospital infections but are responsible for at least 30 percent of the 99,000 annual hospital-infection-related deaths, according to the best estimates available.
Even for those who survive, a central-line infection means weeks or months of debilitating treatments and side effects.
"I certainly did not expect to go through the torture that happened to me," said Carol Bradley, 61, a registered nurse from Nashville, Tenn., who developed several types of infections, including a bloodstream infection, after surgery for stomach cancer in August 2008. As a result, she spent about three weeks in intensive care hooked up to feeding and breathing tubes and central-line catheters, and more than a year on antibiotics.
For decades, doctors considered central-line infections an unavoidable risk of intensive care. But determined reformers have now shown that hospitals can cut their infection rate to zero or close to it by following a low-tech program that includes a simple checklist. Want proof? See our list of hospitals that report zero central-line infections.
Citizen activists across the country, including those working with Consumer Reports, have helped to enact laws in most, states forcing hospitals to publicly disclose their infection rates as a first step, it's hoped, toward improving them. Many of the states have made that information publicly available.
For our analysis, we compared central-line infection data for intensive-care units at over 1,000 hospitals across the country. (Among the nation's roughly 5,000 acute-care hospitals, about 3,300 provide intensive care, but in many, there were too few patients to yield statistically meaningful data, and many are still not reporting publicly.) Our information comes from the state reports and from the Leapfrog Group, a nonprofit organization based in Washington, D.C., that since 2000 has worked with large employers nationwide to collect and disseminate quality information on individual hospitals. The Leapfrog information, which the hospitals submit voluntarily, includes rates of central-line infections in ICUs. Our analysis adjusts for the fact that Leapfrog and the states have data from varying mixtures of ICUs—such as cardiac and surgical—requiring comparisons to different average infection rates.

Most adults have probably had a standard intravenous line at some point in their lives. Central lines are nothing like those.
"When people are as sick as they are in intensive care, you need a way to get things into them in large volumes, and very fast, such as nutrition, fluids or a blood transfusion," explained John Santa, M.D., M.P.H., director of the Consumer Reports Health Ratings Center. "If you put medication into a central line, it gets into the system much faster than if you put it into a regular IV."
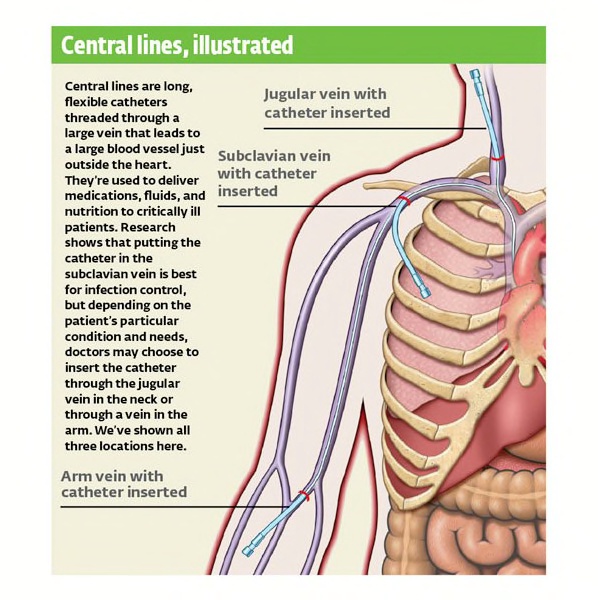
The lines are long, flexible catheters that thread through a large vein that leads to the heart. Unlike regular IVs, which usually stay in for only a few days, central lines can stay put for weeks or even months. It's not unusual for a patient to have something put into a central line many times a day.
The problem is that every time a doctor, nurse, or medical technician touches that line or the skin surrounding it, or the catheter's dressing is dislodged, there's a risk of introducing bacterial contamination unless the strictest sterile conditions are observed. If that happens, the central line's biggest virtue—the ability to spread its cargo throughout the body quickly—becomes its biggest vice. Bacteria, including the antibiotic-resistant "superbugs" present in most hospitals, can quickly multiply, causing sepsis, an infection of the entire bloodstream.
"Sepsis produces high fevers, rigors—violent shaking chills—and the high fever could induce delirium," says Peter Pronovost, M.D., Ph.D., critical-care specialist at the Johns Hopkins School of Medicine in Baltimore. "Imagine the worst you ever felt from the flu, multiplied by 10."
And it is deadly: Sepsis kills up to 50 percent of its victims.
Pearl Gelman, 91, was admitted to a Florida hospital in May 2007 with bronchitis symptoms, according to her daughter, Susan Denenberg of Merrick, N.Y. "She couldn't get antibiotics through her arms because the veins were very bad," Denenberg said. "That's why they had to do it through the neck." Later, she said, the hospital called for permission to replace the central line. "She was getting weaker and weaker, and then they told us she had the MRSA," Denenberg said, referring to the superbug methicillin-resistant staphylococcus aureus. "And it was just downhill. She couldn't fight back. She died at the hospital."
The way hospitals think about central-line infections has changed in recent years, said James J. Gordon, M.D., chief of infectious diseases at Huron Valley-Sinai Hospital in Commerce, Mich. "If best practices are utilized, the vast majority of line infections can be avoided," he said. Medicare agrees: It no longer pays the extra costs associated with those infections.
The breakthrough came after years of research on effective steps in infection control, when Peter Pronovost, M.D.,Ph.D., of Johns Hopkins implemented this body of evidence in the unlikely form of a simple five-step checklist. The checklist translated the most effective known approaches into a common-sense series of precautions to follow when inserting, using, or removing a central line.
The steps require equipment no more complex than hand soap, an antiseptic solution, and sterile drapes and garb. Other key components: giving nurses the authority to make doctors follow all the steps, and measuring and reporting infection rates.
Research suggests that the checklist can cut infections linked to central lines by two thirds, and save thousands of lives and millions of dollars.
Though the checklist seems simple, it does demand time and attention in the high-pressure environment of an ICU.
We now have Ratings on central-line bloodstream infections for 1,068 hospitals nationwide. Of those, 138 (13 percent) reported zero infections. That's slightly more than last year, when 11 percent reported zero infections. Most impressive of all are the 30 hospitals that reported zero central-line bloodstream infections in at least 1,000 central-line days in both our February 2010 and September 2011 releases. For detailed information on the hospitals listed below, as well as others you're interested in, use our hospital Ratings. (Hospitals are listed alphabetically by state.)
| Hospital | City and State |
|---|---|
| Fresno Medical Center | Fresno, Calif. |
| John F. Kennedy Memorial Hospital | Indio, Calif. |
| Marin General Hospital | Greenbrae, Calif. |
| Presbyterian Intercommunity Hospital | Whittier, Calif. |
| Saint Francis Memorial Hospital | San Francisco, Calif. |
| Santa Rosa Medical Center | Santa Rosa, Calif. |
| St. Mary's Medical Center | San Francisco, Calif. |
| Sutter Coast Hospital | Crescent City, Calif. |
| Huron Valley-Sinai Hospital | Commerce Township, Mich. |
| MidMichigan Medical Center-Midland | Midland, Mich. |
| Northern Michigan Regional Hospital | Petoskey, Mich. |
| Children's Hospitals and Clinics of Minnesota | Minneapolis, Mn. |
| Phelps County Regional Medical Center | Rolla, Mo. |
| Southern Hills Hospital and Medical Center | Las Vegas, Nv. |
| Cayuga Medical Center at Ithaca | Ithaca, N.Y. |
| Glen Cove Hospital | Glen Cove, N.Y. |
| Rome Memorial Hospital | Rome, N.Y. |
| Saratoga Hospital | Saratoga Springs, N.Y. |
| Vassar Brothers Medical Center | Poughkeepsie, N.Y. |
| Southern Ohio Medical Center | Portsmouth, Ohio |
| Bon Secours St. Francis Health System | Greenville, S.C. |
| Indian Path Medical Center | Kingsport, Tenn. |
| Texas Health Harris Methodist Hospital Hurst-Euless-Bedford | Bedford, Texas |
| Texas Health Harris Methodist Hospital Southwest Fort Worth | Fort Worth, Texas |
| Timpanogos Regional Hospital | Orem, Utah |
| Inova Alexandria Hospital | Alexandria, Va. |
| Inova Loudoun Hospital | Leesburg, Va. |
| Kadlec Medical Center | Richland, Wash. |
| Northwest Hospital and Medical Center | Seattle, Wash. |
| Saint Clare's Hospital | Weston, Wis. |
Sources: Public state infection reports and the Leapfrog Group.
One of the most important things to know about a hospital is how many of its patients develop central-line bloodstream infections. But many hospitals don't release that information, even though all can do so if they choose. To help motivate them, we put together a list of leading academic hospitals—facilities that should know better—that don't make information on central-line bloodstream infections easily accessible.
"The best hospitals know that sunlight is the best disinfectant, so they are willing to publicly report even if their performance is not yet optimal," said Leah Binder, chief executive officer of The Leapfrog Group, a nonprofit organization that focuses on improving health care in hospitals, in part by encouraging them to report information on infections and other measures.
The table below includes teaching hospitals (excluding Veterans Administration hospitals) that aren't required to provide their data to state-run databases and haven't voluntarily released the information to Leapfrog. The list is arranged alphabetically by state.
You can also use our hospital Ratings to see how well hospitals in your area performed in preventing bloodstream infections. If a hospital doesn't have a Rating in that measure, in means either that they haven't reported the information, or reported it in way that we couldn't use. For those hospitals, you should ask hospitals directly for the information. If they can't or won't give it to you, either no one is keeping track or they don't think you need to know—neither of which is a good sign.
| Hospital* | City, State |
|---|---|
| University of Alabama Hospital | Birmingham, AL |
| University of South Alabama Medical Center | Mobile, AL |
| Arkansas Children's Hospital | Little Rock, AR |
| UAMS Medical Center | Little Rock, AR |
| Maricopa Integrated Health System | Phoenix, AZ |
| TMC Healthcare | Tucson, AZ |
| University Medical Center | Tucson, AZ |
| George Washington University Hospital | Washington, DC |
| Georgetown University Hospital | Washington, DC |
| Howard University Hospital | Washington, DC |
| Washington Hospital Center | Washington, DC |
| All Children's Hospital | Saint Petersburg, FL |
| Florida Hospital | Orlando, FL |
| H. Lee Moffitt Cancer Center and Research Institute | Tampa, FL |
| Jackson Health System | Miami, FL |
| Mount Sinai Medical Center | Miami Beach, FL |
| Shands at the University of Florida | Gainesville, FL |
| Shands Jacksonville Medical Center | Jacksonville, FL |
| Tampa General Hospital | Tampa, FL |
| Children's Healthcare of Atlanta | Atlanta, GA |
| Emory University Hospital | Atlanta, GA |
| Emory University Hospital Midtown | Atlanta, GA |
| Grady Memorial Hospital | Atlanta, GA |
| Medical Center of Central Georgia | Macon, GA |
| Medical College of Georgia Health | Augusta, GA |
| Iowa Methodist Medical Center | Des Moines, IA |
| University of Iowa Hospitals and Clinics | Iowa City, IA |
| Ball Memorial Hospital | Muncie, IN |
| Clarian Health Partners | Indianapolis, IN |
| Wishard Health Services | Indianapolis, IN |
| The University of Kansas Hospital | Kansas City, KS |
| University of Kentucky Albert B. Chandler Hospital | Lexington, KY |
| University of Louisville Hospital | Louisville, KY |
| Medical Center of Louisiana at New Orleans | New Orleans, LA |
| Ochsner Medical Center | New Orleans, LA |
| Ochsner Medical Center - Kenner | Kenner, LA |
| Our Lady of the Lake Regional Medical Center | Baton Rouge, LA |
| Touro Infirmary | New Orleans, LA |
| National Institutes of Health Clinical Center | Bethesda, MD |
| Henry Ford Hospital | Detroit, MI |
| Hurley Medical Center | Flint, MI |
| Ingham Regional Medical Center | Lansing, MI |
| McLaren Regional Medical Center | Flint, MI |
| Oakwood Hospital & Medical Center-Dearborn | Dearborn, MI |
| Abbott Northwestern Hospital | Minneapolis, MN |
| Hennepin County Medical Center | Minneapolis, MN |
| University of Minnesota Medical Center, Fairview | Minneapolis, MN |
| Methodist Rehabilitation Center | Jackson, MS |
| University Hospitals and Health System, University of Mississippi Medical Center | Jackson, MS |
| Carolinas Medical Center | Charlotte, NC |
| Duke University Hospital | Durham, NC |
| Pitt County Memorial Hospital | Greenville, NC |
| MeritCare Medical Center | Fargo, ND |
| University of New Mexico Hospitals | Albuquerque, NM |
| Hospital for Joint Diseases at NYU Lagone Medical Center | New York, NY |
| Hospital for Special Surgery | New York, NY |
| Children's Medical Center | Dayton, OH |
| Cleveland Clinic Foundation | Cleveland, OH |
| Good Samaritan Hospital | Cincinnati, OH |
| Kettering Medical Center | Kettering, OH |
| MetroHealth Medical Center | Cleveland, OH |
| Northside Medical Center | Youngstown, OH |
| St. Elizabeth Health Center | Youngstown, OH |
| Summa Health System | Akron, OH |
| The University of Toledo Medical Center | Toledo, OH |
| University Hospital | Cincinnati, OH |
| Albert Einstein Medical Center | Philadelphia, PA |
| Crozer-Chester Medical Center | Upland, PA |
| Fox Chase Cancer Center-American Oncologic Hospital | Philadelphia, PA |
| Geisinger Medical Center | Danville, PA |
| Hospital of the University of Pennsylvania | Philadelphia, PA |
| Lankenau Hospital | Wynnewood, PA |
| Magee-Womens Hospital of UPMC | Pittsburgh, PA |
| Penn State Milton S. Hershey Medical Center | Hershey, PA |
| St. Luke's Hospital - Bethlehem Campus | Bethlehem, PA |
| Temple University Hospital | Philadelphia, PA |
| Thomas Jefferson University Hospital | Philadelphia, PA |
| UPMC Mercy | Pittsburgh, PA |
| UPMC Presbyterian | Pittsburgh, PA |
| Western Pennsylvania Hospital | Pittsburgh, PA |
| York Hospital | York, PA |
| Women & Infants Hospital of Rhode Island | Providence, RI |
| Avera McKennan Hospital and University Health Center | Sioux Falls, SD |
| Sanford University of South Dakota Medical Center | Sioux Falls, SD |
| Children's Medical Center of Dallas | Dallas, TX |
| Harris County Hospital District | Houston, TX |
| JPS Health Network | Fort Worth, TX |
| Medical Center Hospital | Odessa, TX |
| Memorial Hermann - Texas Medical Center | Houston, TX |
| Parkland Health & Hospital System | Dallas, TX |
| Scott and White Memorial Hospital | Temple, TX |
| St. Luke's Episcopal Hospital | Houston, TX |
| University Health System | San Antonio, TX |
| University Medical Center | Lubbock, TX |
| University Medical Center of El Paso | El Paso, TX |
| University of Texas M.D. Anderson Cancer Center | Houston, TX |
| University of Texas Medical Branch Hospitals | Galveston, TX |
| University of Utah Health Care - Hospital and Clinics | Salt Lake City, UT |
| Aurora Sinai Medical Center | Milwaukee, WI |
| Aurora St. Luke's Medical Center | Milwaukee, WI |
| Froedtert Memorial Lutheran Hospital | Milwaukee, WI |
| Gundersen Lutheran Medical Center | La Crosse, WI |
| University of Wisconsin Hospital and Clinics | Madison, WI |
| Charleston Area Medical Center | Charleston, WV |
| West Virginia University Hospitals | Morgantown, WV |
All hospitals are members of the Council of Teaching Hospitals.
Sources: Public state infection reports and the Leapfrog Group.

A program that includes this checklist has been proved to prevent infections acquired in the hospital from central-line catheters, and probably helps save lives, too. But not all hospitals have adopted it. If a family member or friend has to be hospitalized in intensive care, take this list with you and ask whether the intensive-care unit uses it, says checklist developer Peter Pronovost, M.D., Ph.D., critical-care specialist and patient-safety researcher at the Johns Hopkins School of Medicine.
Caregivers should:
The first step in preventing hospital infections is using our Hospital Ratings to see whether hospitals in your area have made their infection rates public and, if so, trying to choose one with lower rates. If you don't have a choice, you can at least see how your hospital performs and, if it's not good, prepare yourself for being in aggressive in monitoring infection-control practices.
Specifically, patients, friends, and family members should insist that caregivers:
 Build & Buy Car Buying Service
Build & Buy Car Buying Service
Save thousands off MSRP with upfront dealer pricing information and a transparent car buying experience.
 Get Ratings on the go and compare
Get Ratings on the go and compare
while you shop