Sign In


Inhaled steroids reduce and prevent inflammation, swelling, and mucus build-up in your airways and lungs to help prevent asthma attacks and help you breathe easier.
But not everyone with asthma needs an inhaled steroid. Sometimes lifestyle adjustments— including quitting smoking and avoiding exposure to asthma triggers, such as pet dander or mold—work well enough. On the other hand, many people who could benefit from an inhaled steroid don't use one of these medicines. So if your asthma symptoms are persistent and you have frequent asthma attacks, talk to your doctor about an inhaled steroid.

Taking effectiveness, safety, and cost into account, we have chosen the following steroid inhalers as our Best Buys for treating adult and childhood asthma.
■ Beclomethasone (QVAR): For adults and children ages 5 years and older.
■ Generic budesonide suspension nebulizer: For children ages 1 year and older.
Beclomethasone (QVAR) is as effective and safe as other inhaled steroids, and it is the least expensive, ranging from $142 to $177 per month, depending on dose. But if you or your child needs a higher strength to control asthma symptoms, that can increase the cost. If an inhaled steroid does not help or does not relieve your symptoms enough, current guidelines from the National Heart, Lung, and Blood Institute recommend adding a long-acting bronchodilator, such as salmeterol (Serevent Diskus) or formoterol (Foradil), so ask your doctor if that makes sense in your case.
We chose generic budesonide suspension nebulizer for children ages 1 year or older because it is the only inhaled steroid FDA-approved for kids that young. You could save up to $168 by taking the generic version instead of the brand-name counterpart, Pulmicort Respules. But the generic is not available at the highest dose (1 mg/2 mL), so if your child needs a dose that high, you will have to opt for the brand name Pulmicort Respules, which is very expensive at a retail price of $778 per month.

Asthma is a chronic disease that causes inflammation or narrowing of the airways that carry the air you breathe in and out of your lungs. This can make it difficult to breathe and lead to wheezing (noisy breathing), coughing, shortness of breath, and a sensation of tightness in the chest.
About 25 million Americans, including seven million children, have asthma, according to the National Heart, Lung, and Blood Institute. The disease usually first appears in childhood but adults can also develop it.
In treating asthma, inhaled steroids are favored over steroid pills because they act directly on the airways. This enhances their effectiveness and allows a lower dose to be used. The lower dose of an inhaled steroid, compared to steroid pills, lowers the risk of side effects.
Asthma symptoms can be caused by exposure to common allergens (such as animal dander, dust mites, and pollen) and irritants (such as certain chemicals, tobacco or wood smoke, and even cold air). Strenuous exercise, the common cold and the flu, certain drugs—such as aspirin and ibuprofen—and stress can also cause asthma attacks.
For people with asthma, the allergens, irritants, or conditions listed can cause inflammation in the walls of the airways and make the muscles around the airways spasm. This constricts the airways and causes increased mucus production, both of which make it difficult for air to move in and out of the lungs.
Asthma symptoms range from mild to severe and doctors classify people with asthma according to the frequency and severity of their symptoms. The severity of your symptoms can vary; on some days they may be more severe than on others.

Your doctor will first want to rule out other causes of your symptoms and then assess how severely you are affected. That will help determine your treatment, including the drugs you may need.
In addition to questions about your medical history, symptoms, and lifestyle habits, you are likely to undergo tests of your lung function. For example, a spirometry test measures lung capacity by assessing how much and how fast you can blow air out of your lungs after you take a deep breath. During the test, the doctor may also give you an inhaled bronchodilator to see if it helps your lungs function better. If it does, that's an indication that you have asthma.
Asthma can usually be controlled with treatment. Most people with asthma lead normal active lives and having asthma doesn't change how long they will live. But if left untreated, severe asthma symptoms can require emergency treatment or even be deadly. On average, nine people die from asthma every day, and 1.9 million visit a hospital emergency room each year because of an asthma attack, according to the Centers for Disease Control and Prevention.
| Degree | Severity and frequency of symptoms |
| Intermittent | Your asthma comes and goes, with symptoms either during the day or night, occurring twice a week or less. In between, you have no symptoms and your lung function is normal. |
| Mild Persistent | You have symptoms more than twice a week, but not every day. Symptoms at night usually occur more than twice a month and asthma attacks might somewhat limit your activity. |
| Moderate Persistent | You have symptoms every day and/or you have night symptoms more than once a week. The attacks limit your activity. |
| Severe Persistent | You have symptoms throughout the day, most days. Symptoms often come at night as well. Activity is extremely limited. |
Source: National Heart, Lung, and Blood Institute, National Asthma Education and Prevention Program. Expert panel report 3: Guidelines for the diagnosis and management of asthma. August 2007

An important part of keeping your asthma symptoms under control is to figure out what your triggers are and avoid them. The chart shown above lists some common triggers and steps you can take to avoid or reduce your exposure. In some cases, allergy skin testing can help you identify your triggers.
Other things than can make asthma worse include sulfites in foods and beverages. These are commonly found in beer, wine, dried fruit, processed potatoes, and shrimp, so avoid those if they cause asthma attacks.
For some people, cold air can be a trigger, so in that case, covering your nose and mouth with a scarf on cold days can help.
Medications, such as aspirin, ibuprofen, and other non-steroidal anti-inflammatory drugs or NSAIDs, can also cause attacks, so discuss with your doctor all the prescription and over-the-counter medications, vitamins, and dietary supplements you take.
One trigger you should not avoid is exercise. Although it can cause an attack (known as exercise-induced bronchospasm), exercise is an important part of a healthy lifestyle. If it's difficult for you to exercise because it induces asthma symptoms, talk to your doctor about ways you can stay active. People with asthma might benefit from using their quick-acting inhaler medicine before exercise.
If an asthma attack makes you so short of breath that you're having trouble walking and talking or your lips or fingernails turn blue, call 911. You may need emergency care at a hospital.
Many people try alternative therapies for asthma, such as acupuncture, diets, herbs or vitamins, and homeopathic remedies. Very little research has been done on those treatments but the available studies indicate they are ineffective. And some—such as herbal ephedra—can be dangerous. The FDA has now banned ephedra.
Asthma trigger |
Avoiding the triggers |
| Pet/animal dander | • Keep pets out of your home, room or living area |
| Dust mites (tiny bugs found in every home, especially in mattresses, pillows, carpets, and upholstered furniture) | • Buy a dust-proof cover for your mattress and pillows • Wash pillows, sheets, and blankets each week in hot water (or cold water with detergent and bleach) • Don't keep stuffed toys on the bed or wash them each week |
| Cockroaches | • Food can attract cockroaches, so store it in closed containers and use closed garbage cans • Use roach traps, baits or sprays |
| Indoor mold | • Clean moldy areas with a cleaner that contains bleach • Fix leaky faucets or pipes that have mold around them |
| Pollen and outdoor mold | • During allergy season, keep windows closed and stay indoors from late morning to afternoon if possible |
| Tobacco smoke | • If you smoke, quit or ask your doctor about strategies that can help you quit • Don't allow smoking in your home or car |
| Other types of smoke, strong odors, and sprays | • Don't use a wood-burning stove, kerosene heater, or fireplace, if possible • Avoid perfumes, talcum powder, hair sprays, and paints |
| Vacuum cleaning | • Have someone else vacuum for you and stay out of areas while they are being vacuumed • If you have to vacuum, use a dust mask, a double-layered or microfilter vacuum cleaner bag, or a HEPA filter |
Source: National Heart, Lung, and Blood Institute
Inhaled steroids are generally recommended as the first option for the treatment of persistent asthma symptoms in adults and children. This report focuses on the six inhaled steroid medicines that are available by prescription in the U.S. They are:
| Generic name | Brand name(s) | Available as a generic drug? |
| Beclomethasone | QVAR | No |
| Budesonide | Pulmicort Flexhaler | No |
| Pulmicort Respules | Yes | |
| Ciclesonide | Alvesco | No |
| Flunisolide | Aerospan (Approved by the FDA but not on the market yet) |
No |
| Fluticasone | Flovent HFA, Flovent Diskus |
No |
| Mometasone | Asmanex Twisthaler |
No |
Other medicines and approaches are used to treat asthma. They include:
Quick-relief inhalers: All people with asthma should have a "quick relief" inhaler (also known as a short-acting inhaled beta 2-agonist, or SABA). These inhalers—which include albuterol (Proair HFA, Ventolin HFA) and levalbuterol (Xopenex)—act rapidly—within minutes—to open breathing passages, and provide relief for up to six hours. They are only used during an attack when breathing might be very difficult, and not—like inhaled steroids—everyday to keep symptoms and attacks at bay and your airways open.
Long-acting bronchodilators. Known as long-acting inhaled beta 2-agonists, or LABAs, these can improve breathing for up to 12 hours. But they have been linked to a higher risk of death during asthma attacks. They now carry a black box warning—the strongest kind—that they should only be used in people whose asthma is not adequately controlled by inhaled steroids alone. The LABAs should never be used without also using an inhaled steroid.

Two LABAs are available: salmeterol (Serevent Diskus) and formoterol (Foradil and Perforomist). Three other products combine these long-acting relievers with inhaled steroids: Advair Diskus and Advair HFA (both include a combination of salmeterol and fluticasone), Symbicort (a combination of budesonide and formoterol), and Dulera (a combination of mometasone and formoterol).
If your doctor prescribes any of the LABAs or combination products that contain a LABA, we urge you to discuss with him or her the safety issues that have been raised about those medications.
Medication in pill form. If you have asthma your doctor may prescribe a type of drug called a leukotriene receptor antagonist or LTRA, such as montelukast (Singulair and generic) or zafirlukast (Accolate and generic). There's good evidence that these drugs work, but they are not considered to be as effective as inhaled steroids at reducing the severity of symptoms or the frequency of asthma attacks.
But some evidence shows that people find it easier to regularly take a pill than to use an asthma inhaler on a daily basis. Two 2-year trials found that the LRTAs were just as effective as the inhaled steroids, primarily because more people—65 percent and 74 percent—in the LRTA groups took their medicine every day compared with only 41 percent and 46 percent of those in the inhaled steroid group.
Your medication can't work if you don't take it, so if you find that it is difficult to use an inhaler every day, tell your doctor so he or she can help you find a strategy you can stick with.

A ban on the propellant once used in inhalers is partially to blame for the dramatic price increases in the last few years. In 2010, the Food and Drug Administration required manufacturers of inhalers to stop using chlorofluorocarbon propellants because they posed a threat to the environment. In response, the manufacturers developed new inhalers with new patents. This has delayed generics from entering the market. Without that competition, the manufacturers have been able to increase the price—an average of 50 percent since 2009, with some medications jumping 80 percent or more in price.
For example, QVAR 80 mcg, at $177 for a month's supply, is 92 percent more expensive than it was in 2009, according to prices from Symphony Health Solutions, which is not involved in our analysis or recommendations. Pulmicort nebulizer is another example. Over the last five years, the monthly price has jumped as high as 86 percent. Even the price of budesonide, the only generic inhaled steroid currently available, has risen 47 percent over the last three years.
When the patents on the new inhalers expire, that would open the way for less costly generics. That would, in turn, help drive down the prices of inhaled steroids across the board. But it's unclear when additional generics besides budesonide will become available.
In the meantime, people with limited or no drug coverage under their insurance plan could save money by shopping around in their area. Call your local pharmacies and ask for the lowest available price or the best deal they can offer. Don't leave out independent pharmacies. Our secret shoppers recently found that they sometimes have the lowest prices (and sometimes the highest, too), so it's worth a call to find out. Other less-expensive pharmacies can include Costco and Walmart, and two U.S. websites, FamilyMeds.com and Healthwarehouse.com.
Inhaled steroids reduce and prevent inflammation, swelling, and mucus buildup in your airways and lungs. By doing so, they help prevent asthma attacks and keep you breathing easier, allowing an adequate amount of oxygen to get into your lungs and then your bloodstream. So they help relieve symptoms, but they are not a cure for asthma.
Everyone with asthma should have readily available a "quick relief" inhaler (or SABA), but not everyone with asthma needs an inhaled steroid drug. Sometimes, lifestyle adjustments, including quitting smoking and avoiding exposure to triggers, such as pet dander or mold, work well enough that an inhaled steroid isn't necessary. But most people with asthma—including children—will probably need some kind of controller medicine, and an inhaled steroid drug in particular.
If you or your child has persistent asthma—attacks or symptoms more than twice a week, or attacks that interfere with normal activity—your doctor is very likely to prescribe an inhaled steroid. Even with mild symptoms, your doctor is likely to advise using an inhaled steroid to help prevent them.
If you have only intermittent and/or mild attacks that don't really interfere with leading a normal life, your doctor may suggest that you try to control the symptoms with a fast-acting reliever as needed, and not take an inhaled steroid unless your symptoms worsen. One sign of that would be if you find that you are using your quick-relief inhaler more than two times a week.
Children usually need lower doses of asthma drugs than adults. It's important therefore to know the dose of an inhaled steroid that is right for your child.

The inhaled steroids used to treat asthma are not the same as the anabolic steroids that some bodybuilders and athletes use and abuse to enhance performance or strength. So the inhaled steroids don't pose the risks that have been linked to anabolic steroids, such as breast growth and shrinking of testicles in men, voice deepening and growth of body hair in women, heart problems, liver disease, and aggressive behavior.
You may also have heard that taking steroids can stunt your child's growth, but if there is an effect, it's small. Long-term studies show that inhaled steroids can slow growth in children in the first year of treatment. A 2013 study found that this may reduce ultimate adult height slightly—by 1.2 cm on average, but other studies have not found a height reduction. On the other hand, untreated asthma has been shown to stunt a child's growth.
All that said, doctors advise that children always use as low a dose of inhaled steroids as possible.
Various inhaled steroids have been compared against each other in 51 studies that looked at the following criteria.
■ How well did it improve symptoms?
■ How often did it reduced attacks?
■ How often did it reduce the need for short-acting medications or oral steroids?
■ How much did it improve lung function?
■ Did it improve quality of life?
Overall, all inhaled steroids work well in reducing asthma symptoms and preventing asthma attacks, based on those criteria. None have been shown to be consistently better than the others in treating asthma in adults or children.
Some studies found statistically significant differences for some of the above criteria. When there was a difference, fluticasone (Flovent Diskus) was usually found to be somewhat more effective. But in some of those studies, Flovent was given in a stronger dose.
Generic name (Brand name) |
Effective for asthma prevention in adults |
Effective for asthma prevention in children |
Beclomethasone (QVAR) |
Yes | Yes, in children ages 5 years and older |
Budesonide (Pulmicort Flexhaler) |
Yes | Yes, in children ages 6 years and older |
Budesonide (Pulmicort Respules) |
Yes | Yes, in children ages 1 year and older |
Ciclesonide (Alvesco) |
Yes | Yes, in children ages 12 years and older |
Flunisolide (Aerospan HFA) (Not currently available) |
Yes | Yes, in children ages 6 years and older |
Fluticasone (Flovent HFA) |
Yes | Yes, in children ages 4 years and older |
Mometasone (Asmanex Twisthaler) |
Yes | Yes, in children ages 4 years and older |
Of course, as with all medicines, you or your child may respond better to one inhaled steroid than another, or experience fewer side effects with one. Your doctor can help you determine if a particular medication is working for you or not.
The strength and potency of each medicine is different. That means that the dose you may need and the number of puffs you may have to take each day could vary quite widely from drug to drug.
Like most medicines, the inhaled steroids can cause side effects (See Table 3). The most common are mouth and throat irritation, cough, and hoarseness. Those are usually minor and tolerable.
Other side effects include mouth or throat infections (called thrush or oropharyngeal candidiasis). Using a spacer device and thoroughly rinsing your mouth with water after each inhaler use might reduce the risk of these infections.
Some studies have linked inhaled steroids to an increased risk of osteoporosis, or weakening of the bones. But experts continue to debate whether this research is valid and many studies have found no link between using inhaled steroids and loss of bone density or an increased risk of bone fractures. Still, if you are over 50 and use inhaled steroids, you should discuss with your doctor whether to take calcium and vitamin D supplements and have occasional bone density measurements as a precaution.
There have been reports of eye problems, including glaucoma and cataracts, reported in people who had taken high doses of inhaled steroids for a long time. Tell your doctor if you have previously had those conditions or notice a change in your vision while taking an inhaled steroid.
Table 3. Possible side effects of inhaled steroids |
| Minor: Usually go away in time or are short-lived |
■ Cough ■ Headache ■ Hoarseness, sore throat ■ Mouth or throat infection ■ Mouth or throat irritation ■ Nausea or vomiting |
| Serious: These are rare but can be dangerous |
■ Possible eye problems (associated with long-term use) - Glaucoma, cataracts ■ Possible bone thinning |
| More common in older people: These particularly affect women, but they are not dangerous |
■ Thinning of skin ■ Bruising |
Some inhaled steroids can interact with certain antifungal drugs, such as ketoconazole, and HIV medications. So, be sure to tell your doctor about any medications or supplements you take.
The effectiveness of inhaled steroids in treating asthma does not appear to differ based on age, sex, or race, or in people who have other diseases.
In five studies that compared inhaled steroids in children and teens with asthma, the effectiveness was the same as in adults. There have been no studies in children younger than 6 months. Most studies conducted in younger children—under 4 years—only compared budesonide to placebo, so there is little data on other inhaled steroids in young children.
Budesonide (Pulmicort Respules) is the only inhaled steroid that has been proven effective in children as young as 1 year. Budesonide (Pulmicort Flexhaler) is FDA-approved for children 6 years and older. Fluticasone and mometasone are FDA-approved for use in children 4 years and older, and QVAR is approved for children 5 and older.)
All of the inhaled steroids, except budesonide, have been linked to birth defects in animal studies when given during pregnancy, but there is limited information available about the effect of these medications in pregnant women. So inhaled steroids should only be used during pregnancy if the beneficial effects are believed to outweigh the potential harms.
Poorly controlled asthma during pregnancy—which could lead to lower oxygen levels in your blood and for your baby—has been associated with higher rates of premature birth, lower birth weight, and prenatal death. Proper use of inhaled steroids is thought to reduce the potential for those problems. So if you are pregnant and have asthma, ask your doctor whether you should continue to take your inhaled steroid.
Pregnancy increases the production of corticosteroids in the body, so some women may be able to use a lower dose of inhaled steroid while pregnant or stop using the medication.

Taking effectiveness, safety, and cost into account, we have chosen the following steroid inhalers as our Best Buys for treating adult and childhood asthma:
■ Beclomethasone (QVAR)—for adults and children ages 5 years and older
■ Generic budesonide suspension nebulizer—for children ages 1 year and older
Beclomethasone (QVAR) is as effective and safe as other inhaled steroids, and it is the least expensive, ranging from $142 to $177 per month, depending on dose. But if you or your child needs a higher strength to control asthma symptoms, that can increase the cost.
We chose generic budesonide suspension nebulizer for children 1 year or older because it is the only inhaled steroid FDA-approved for children that young. Using the generic could save you between $98 and $168 when compared to its brand-name counterpart, Pulmicort Respules. But the generic is not available at the highest dose (1 mg/2 mL), so if your child needs a dose that high, you will have to opt for the brand name Pulmicort Respules, which is very expensive at a retail price of $778 per month.
How many puffs per day will you need? For instance, beclomethasone (QVAR) has a relatively low potency and, depending on the severity of your condition, it could take four to 16 puffs per day to get the required dose. By comparison, mometasone (Asmanex Twisthaler), which is more potent, requires only one to three puffs per day for an adult (See Table 4, below). For someone who needs a relatively high dose, a drug that requires you to take many puffs per day is inconvenient and may lower the benefit they can get from the drug.
Which inhaler device do you prefer? Four of the medications—beclomethasone (QVAR), ciclesonide (Alvesco), flunisolide, and fluticasone (Flovent HFA)—are available in metered dose inhalers, also known as "puffers." Three—budesonide (Pulmicort Flexhaler), fluticasone (Flovent Diskus) and mometasone (Asmanex Twisthaler)—are available as dry powder inhalers. And budesonide (Pulmicort Respules) is available as a nebulizer, which is used mostly for children. Your doctor can explain the differences and the pros and cons of each.
Whichever type you choose, it is very important that you learn to use your inhaler properly. Studies have shown that many people don't learn this and, as a result, don't get optimal asthma control.
How much does it cost? It can get expensive if you are paying out of your own pocket, or even if your drug costs are covered by insurance. Your insurer may have chosen one of the inhaled steroids as a preferred drug, which could mean a lower cost for you. Unless your doctor recommends a particular inhaled steroid for effectiveness, safety or convenience reasons, you or your child may be best off using the one your health plan prefers if it will cost you less.

Our evaluation is primarily based on an independent scientific review of the evidence on the effectiveness, safety, and adverse effects of the inhaled steroids. A team of physicians and researchers at the Pacific Northwest Evidence-Based Practice Center (EPC) conducted the analysis. A synopsis of that forms the basis for this report. A consultant to Consumer Reports Best Buy Drugs is also a member of the Pacific Northwest EPC research team, which has no financial interest in any pharmaceutical company or product.
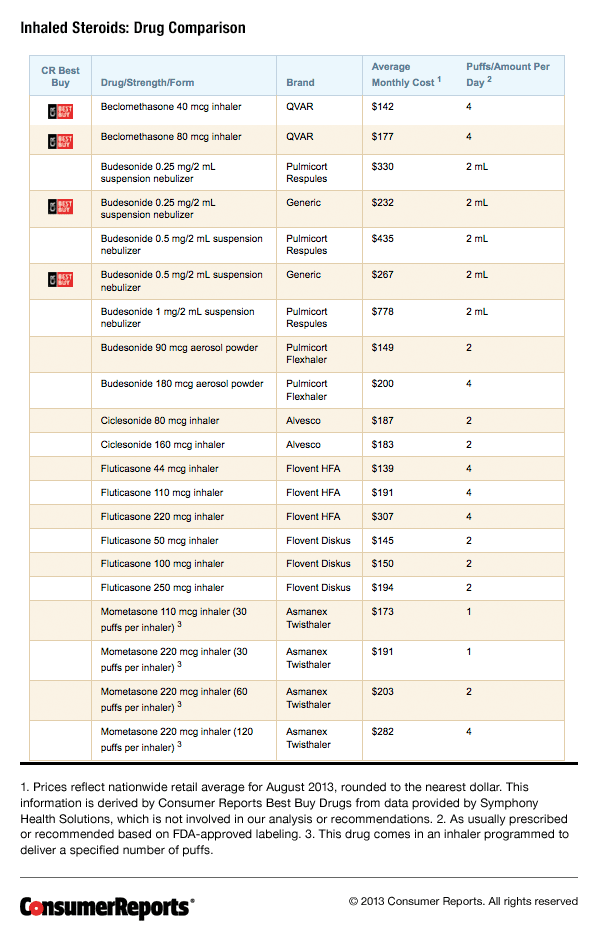
The drug costs we cite were obtained from a healthcare information company which tracks the sales of prescription drugs in the U.S. Prices for a drug can vary quite widely, even within a single city or town. All the prices in this report are national averages based on sales of prescription drugs in retail outlets. They reflect the cash price paid for a month's supply of each drug in August 2013.
We selected the Best Buys using the following criteria. The drug had to:
■ Be approved by the FDA for treating asthma
■ Be as effective as other inhaled steroids
■ Have a safety record equal to or better than other inhaled steroids
■ Have an average price for a 30-day supply that was not higher than the other inhaled steroids
Our methodology is described in more detail in the Methods section at www.CRBestBuyDrugs.org.
1. Adams N. et al., "Fluticasone versus beclomethasone or budesonide for chronic asthma," (Cochrane Review). The Cochrane Library 2004;1.
2. Alsaeedi A. et al. "The effects of inhaled corticosteroids in chronic obstructive pulmonary disease: a systematic review of randomized placebo-controlled trials." Am J Med 2002;113(1):59-65.
3. Banov C. et al., "Budesonide turbuhaler delivered once daily improves health-related quality of life in adult patients with non-steroid-dependent asthma." Allergy Asthma Proc 2003;24(2):129-36.
4. Barnes N.C., et al., "A comparison of fluticasone propionate, 1 mg daily, with beclomethasone dipropionate, 2 mg daily, in the treatment of severe asthma. International Study Group." Eur Respir J 1993;6(6):877-85.
5. Bousquet J. et al., Comparison of the efficacy and safety of mometasone furoate dry powder inhaler to budesonide Turbuhaler." Eur Respir J 2000;16(5):808-16.
6. Burge P.S. et al., "Randomised, double blind, placebo controlled study of fluticasone propionate in patients with moderate to severe chronic obstructive pulmonary disease: the ISOLDE trial." BMJ 2000;320(7245):1297-1303.
7. Calverley P.M. et al., "Maintenance therapy with budesonide and formoterol in chronic obstructive pulmonary disease." Eur Respir J 2003;22(6):912-9.
8. Calverley P. et al., "Combined salmeterol and fluticasone in the treatment of chronic obstructive pulmonary disease: a randomised controlled trial." Lancet 2003;361(9356):449-56.
9. Calverley P.M. et al., "Withdrawal from treatment as an outcome in the ISOLDE study of COPD." Chest 2003;124(4):1350-6.
10. Chervinsky P. Comparison of mometasone furoate administered by metered dose inhaler with beclomethasone dipropionate." Int J Clin Pract 2002;56(6):419-25.
11. Corren J. et al., "Comparison of once-daily mometasone furoate versus once-daily budesonide in patients with moderate persistent asthma." Int J Clin Pract 2003;57(7):567-72.
12. Fabbri L. et al., "Comparison of fluticasone propionate with beclomethasone dipropionate in moderate to severe asthma treated for one year." International Study Group. Thorax 1993;48(8):817-23.
13. Fairfax A. et al., "A randomized, double-blind comparison of beclomethasone dipropionate extrafine aerosol and fluticasone propionate." Ann Allergy Asthma Immunol 2001;86(5):575-82.
14. Fan V.S. et al., "Inhaled corticosteroids in chronic obstructive pulmonary disease and risk of death and hospitalization: time-dependent analysis." Am J Respir Crit Care Med 2003;168(12):1488-94.
15. Hansel TT, Benezet O, Kafe H, et al. A multinational, 12-week, randomized study comparing the efficacy and tolerability of ciclesonide and budesonide in patients with asthma. Clin Ther. Jun 2006;28(6):906-920.
16. Heinig J.H. et al., "The effect of high-dose fluticasone propionate and budesonide on lung function and asthma exacerbations in patients with severe asthma." Respir Med 1999;93(9):613-20.
17. Hoekx J.C. et al., "Fluticasone propionate compared with budesonide: a double-blind trial in asthmatic children using powder devices at a dosage of 400 microg x day(-1)." Eur Respir J 1996;9(11):2263-72.
18. Hubbard R.B., et al., "Inhaled corticosteroids and hip fracture: a population-based case-control study." Am J Respir Crit Care Med 2002;166(12 Pt 1):1563-6.
19. Jones A. et al., "Inhaled corticosteroid effects on bone metabolism in asthma and mild chronic obstructive pulmonary disease." Cochrane Database Syst Rev 2004(1):CD003537.
20. Juniper E.F, et al., "Health-related quality of life in moderate asthma: 400 microg hydrofluoroalkane beclomethasone dipropionate vs 800 microg chlorofluorocarbon beclomethasone dipropionate." The Study Group. Chest 1999;116(5):1297-303.
21. Lee T.A. et al., "Fracture risk associated with inhaled corticosteroid use in chronic obstructive pulmonary disease." Am J Respir Crit Care Med 2004;169(7):855-9.
22. Mahajan P. et al., Impact of fluticasone propionate powder on health-related quality of life in patients with moderate asthma." J Asthma 1997;34(3):227-34.
23. Mahajan P. et al., "The effect of fluticasone propionate on functional status and sleep in children with asthma and on the quality of life of their parents." J Allergy Clin Immunol 1998;102(1):19-23.
24. Medici T.C. et al., "Effect of one year treatment with inhaled fluticasone propionate or beclomethasone dipropionate on bone density and bone metabolism: a randomised parallel group study in adult asthmatic subjects." Thorax 2000;55(5):375-82.
25. Nathan R.A. et al., "Mometasone furoate: efficacy and safety in moderate asthma compared with beclomethasone dipropionate." Ann Allergy Asthma Immunol 2001;86(2):203-10.
26. Newhouse M. et al. "Comparison of efficacy and safety between flunisolide/AeroChamber and budesonide/turbuhaler in patients with moderate asthma." AER-MD-04 Study Group. Ann Allergy Asthma Immunol 2000;84(3):313-9.
27. Paggiaro P.L. et al. "Multicentre randomised placebo-controlled trial of inhaled fluticasone propionate in patients with chronic obstructive pulmonary disease." International COPD Study Group. Lancet 1998;351(9105):773-80.
28. Pauwels R.A. et al., Long-term treatment with inhaled budesonide in persons with mild chronic obstructive pulmonary disease who continue smoking." European Respiratory Society Study on Chronic Obstructive Pulmonary Disease. N Engl J Med 1999;340(25):1948-53.
29. Raphael G.D., et al., "A comparison of multiple doses of fluticasone propionate and beclomethasone dipropionate in subjects with persistent asthma." J Allergy Clin Immunol 1999;103(5 Pt 1):796-803.
30. Ringdal N. et al., "A blinded comparison of fluticasone propionate with budesonide via powder devices in adult patients with moderate to severe asthma: a clinical evaluation." Mediators Inflamm 1996;5:382-89.
31. Sharek P.J. et al., "Beclomethasone for asthma in children: effects on linear growth" (Cochrane Review). The Cochrane Library 2004;1.
32. Simons F.E. "A comparison of beclomethasone, salmeterol, and placebo in children with asthma. Canadian Beclomethasone Dipropionate-Salmeterol Xinafoate Study Group." N Engl J Med 1997;337(23):1659-65.
33. Sin D.D. et al., "Inhaled corticosteroids and the risk of mortality and readmission in elderly patients with chronic obstructive pulmonary disease." Am J Respir Crit Care Med 2001;164(4):580-4.
34. Suissa S. et al. "Low-dose inhaled corticosteroids and the prevention of death from asthma." N Engl J Med 2000;343(5):332-6.
35. Sutherland E.R. et al., "Inhaled corticosteroids reduce the progression of airflow limitation in chronic obstructive pulmonary disease: A meta-analysis." Thorax 2003;58(11):937-941.
36. Szafranski W. et al., "Efficacy and safety of budesonide/formoterol in the management of chronic obstructive pulmonary disease." Eur Respir J 2003;21(1):74-81.
37. Terzano C. et al. "Beclomethasone dipropionate versus budesonide inhalation suspension in children with mild to moderate persistent asthma." Eur Rev Med Pharmacol Sci 2000;4:17-24.
38. Van der Valk P. et al., "Effect of discontinuation of inhaled corticosteroids inpatients with chronic obstructive pulmonary disease: the COPE study." Am J Respir Crit Care Med 2002;166(10):1358-63.
39. Van Grunsven P. et al., "Short- and long-term efficacy of fluticasone propionate in subjects with early signs and symptoms of chronic obstructive pulmonary disease. Results of the DIMCA study." Respir Med 2003;97(12):1303-12.
40. Van Staa T.P. et al., "Use of inhaled corticosteroids and risk of fractures." J Bone Miner Res 2001;16(3):581-8.
41. Vermeulen JH, Gyurkovits K, Rauer H, Engelstatter R. Randomized comparison of the efficacy and safety of ciclesonide and budesonide in adolescents with severe asthma. Respir Med. Oct 2007;101(10):2182-2191.
42. Vestbo J. et al., "Long-term effect of inhaled budesonide in mild and moderate chronic obstructive pulmonary disease: a randomised controlled trial." Lancet 1999;353(9167):1819-23.
43. von Berg A, Engelstatter R, Minic P, et al. Comparison of the efficacy and safety of ciclesonide 160 microg once daily vs. budesonide 400 microg once daily in children with asthma. Pediatr Allergy Immunol. Aug 2007;18(5):391-400.
These materials are made possible by a grant from the state Attorney General Consumer and Prescriber Education Grant Program, which is funded by the multi-state settlement of consumer-fraud claims regarding the marketing of the prescription drug Neurontin (gabapentin).
 Build & Buy Car Buying Service
Build & Buy Car Buying Service
Save thousands off MSRP with upfront dealer pricing information and a transparent car buying experience.
 Get Ratings on the go and compare
Get Ratings on the go and compare
while you shop