Sign In

Injectable drugs referred to as biologic DMARDs (Disease-Modifying Antirheumatic Drugs)—or simply, biologics—are used to treat rheumatoid arthritis, a chronic condition in which the immune system, which normally fights infection, attacks the lining of the joints, causing swelling, stiffness, and pain. If left untreated, it can lead to irreversible joint damage. About 1.3 million adults in the United States suffer from rheumatoid arthritis. It is most common in women, and in people over the age of 40, though it may occur at any age.
The biologics do not cure rheumatoid arthritis, but they do alleviate symptoms and may help prevent further joint damage. However, they can cause serious side effects and should not be used until after you have tried other therapies.
Can glucosamine and chondroitin supplements in liquid form help arthritic joints? Read our Claim Check: Does Joint Juice Work Against Arthrits?
If you have been newly diagnosed with rheumatoid arthritis, studies show that other less costly and safer medications work just as well as biologics, so you should try those first. These include nonbiologic DMARDs, such as hydroxychloroquine (Plaquenil and generic), sulfasalazine (Azulfidine and generic), minocycline (Dynacin, Minocin, and generic), and methotrexate (Rheumatrex and generic). In addition, your doctor is also likely to recommend pain relievers, such as ibuprofen (Advil, Motrin, and generics) and naproxen (Aleve, Naprosyn, and generics), and corticosteroids, such as prednisone. You should also follow an exercise program because studies show such programs improve function in people with rheumatoid arthritis.
If those therapies fail to provide you with enough symptom relief, then it might be time to try a biologic. Between 30 to 70 percent of people who have not benefitted from other rheumatoid arthritis medications experience some measure of relief from biologics. However, people's responses vary—some people symptoms and function improve, while others may not. Roughly 40 percent of people won't respond to any particular treatment, and will probably need to switch to another biologic.
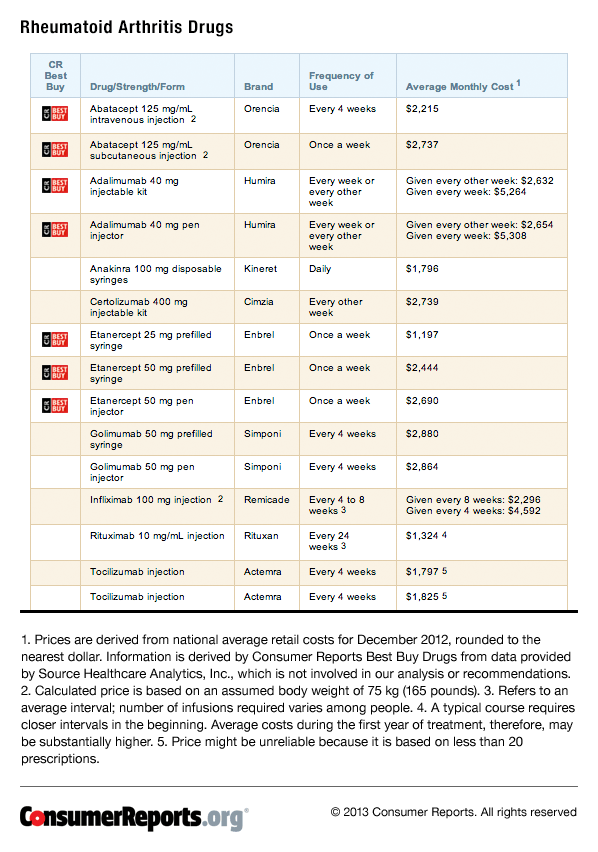
Nine different biologics are available to treat the symptoms of rheumatoid arthritis, but they are not a cure. They are all very expensive, with some costing more than $5,000 per week. Taking into account the evidence for effectiveness and safety, if you need a biologic drug to treat your rheumatoid arthritis, we have chosen the following asConsumer Reports Best Buy Drugs:
■ Abatacept (Orencia)
■ Adalimumab (Humira)
■ Etanercept (Enbrel)
Studies show that these three medications are as effective as the other biologics for relieving rheumatoid arthritis symptoms, and they also may have lower rates of withdrawal due to adverse effects than some other biologics.
All of the biologics can cause side effects. In studies, people who took a biologic had a higher risk—13 percent versus 12 percent—of experiencing a serious life-threatening allergic reaction, infection, lymphoma, or other serious side effect than those who took a placebo. The serious or potentially life-threatening infections include bacterial infections, such as tuberculosis, pneumonia, or staph, and serious fungal infections. Minor side effects, such as abdominal pain, nausea, and injection site reactions, can also occur, but usually do not require stopping or changing drugs.

This analysis is based on a comprehensive expert analysis of the medical evidence on biologics to treat rheumatoid arthritis. The biologics are a type of "Disease-modifying Antirheumatic Drug (DMARD)" that not only treat symptoms, but can also reduce joint and bone damage.
| Generic Name | Brand Name |
| Abatacept | Orencia |
| Adalimumab | Humira |
| Anakinra | Kineret |
| Certolizumab | Cimzia |
| Etanercept | Enbrel |
| Golimumab | Simponi |
| Infliximab | Remicade |
| Rituximab | Rituxan |
| Tocilizumab | Actemra |
All of them are very expensive. A new biologic, Xeljanz (tofacitinib), that is available as a pill, was approved by the FDA in late 2012 for the treatment of rheumatoid arthritis, but it was not included in the analysis that forms the basis of this report so we don't assess how it compares to the other biologics. Xeljanz is associated with perforations in the stomach and intestines, and elevations in cholesterol levels and liver enzymes, so we recommend avoiding it if possible, until more is known about its effectiveness and safety profile.
Biologics are seen as a significant advancement over other drugs used to treat rheumatoid arthritis — for example, methotrexate (Rheumatrex, Trexall, and generic), leflunomide (Arava and generic), hydroxychloroquine (Plaquenil and generic), and sulfasalazine (Azulfidine and generic) — which are often referred to as conventional or nonbiologic
DMARDs. But that said, biologics should only be used if conventional DMARDs do not work well enough for you on their own. Other treatments for rheumatoid arthritis often used with biologics include pain relievers or nonsteroidal anti-inflammatory drugs (NSAIDs) — for example, ibuprofen (Advil, Motrin, and generic) and naproxen (Aleve and generic) — and corticosteroids, such as prednisone. We do not evaluate the conventional DMARDs or other rheumatoid arthritis treatments, or compare them with biologics.
This analysis focuses specifically on the use of biologics used to treat rheumatoid arthritis, though it is worth noting that some of the biologics have multiple uses and are also approved for treating other diseases, such as ankylosing spondylitis, Crohn's disease, psoriasis, and ulcerative colitis.
Biologics work by interfering directly with the human body's immune system, the protective mechanism that fights bacteria and viruses, kills sick cells, and generally helps you stay healthy.
Sometimes, for unknown reasons, the immune system turns against the body and attacks it. This process is called autoimmunity. Rheumatoid arthritis is one of many different autoimmune diseases. In rheumatoid arthritis, the immune system attacks tissue inside the joints, causing inflammation, pain, joint damage, and ultimately joint destruction. By blocking certain components of the immune system, biologics help stop or reduce the inflammation caused by the misdirected attack.
Your doctor should not prescribe a biologic if: |
■ Your rheumatoid arthritis is not active (i.e., your arthritis is in remission) ■ You have not tried a conventional DMARD first ■ You have an infection ■ You have previously had severe reactions to biologics |
Your doctor may decide not to prescribe a biologic if: |
■ You are pregnant or breastfeeding ■ You have had tuberculosis in the past ■ You have had other repeated infections ■ You have had cancer ■ You have or had a serious heart condition ■ You have lung fibrosis |
Rheumatoid arthritis is characterized by pain, swelling, and inflammation of the joints. It most commonly starts in the small joints of the hands and feet. Eventually all joints can be affected. Your joints can feel stiff, particularly in the morning. Symptoms often come and go, and are often accompanied by fever or feeling tired or unwell. As the disease progresses, sufferers can experience severe joint damage and fatigue, making it difficult for them to complete everyday tasks. Flare-ups of rheumatoid arthritis are often unpredictable and difficult to manage. Pain, stiffness, and swelling are worse on some days and easier to bear on others.
The exact cause of rheumatoid arthritis is unknown. Some studies show that rheumatoid arthritis may run in families, suggesting a genetic component, yet having a family member who suffers from rheumatoid arthritis does not necessarily mean that you will also develop the disease.
Rheumatoid arthritis can be difficult to diagnose because many other conditions can cause joint stiffness, pain, swelling, and inflammation.
Your doctor will ask you about your symptoms and run a series of tests to confirm the diagnosis. Common blood tests your doctor might run include rheumatoid factor and anti-CCP antibodies. These are antibodies that eight out of 10 people with rheumatoid arthritis carry in their blood. Both rheumatoid factor and anti-CCP antibodies can also be found in one out of 20 people without rheumatoid arthritis, so these tests cannot confirm rheumatoid arthritis. Other tests include the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). These can help determine the degree of inflammation in your body. Another common test analyzes X-ray images of your hands to identify joint damage.
The type of medication your doctor will consider depends on the severity of your rheumatoid arthritis, the results of blood tests and X-ray images, the length of time that you have been experiencing symptoms, the rate of progression of your symptoms, and other medical problems that you may have. People who are newly diagnosed with rheumatoid arthritis will most likely be started on a pain reliever, corticosteroid, or conventional DMARD, with biologics reserved for second-line therapy if those treatments are not effective.
Some rheumatoid arthritis medications relieve pain, such as ibuprofen (Advil, Motrin, and generics), and naproxen (Aleve, Naprosyn, and generics). Steroids, such as prednisone and methylprednisolone (Medrol), may slow the progression of joint damage, but they do not cure the disease. In addition, your doctor might also prescribe one of the conventional DMARDs, which can help limit joint damage, but also are not a cure. Studies show that for many people, these drugs work just as well as biologics, at a much lower cost.
Exercise can also help. Studies show that exercise programs improve the function of people with rheumatoid arthritis. These programs are typically recommended as a complement to, not a replacement for, medications.
If your symptoms continue to progress despite participation in an exercise program and the use of other rheumatoid arthritis medications, such as the conventional DMARDs, or if you experience intolerable side effects from these drugs, your doctor may suggest a biologic. But you should be aware that these can cause rare, but serious side effects, including infections that require a hospital stay, tuberculosis, nonmalignant skin cancer and lymphoma, and allergic reactions following infusion (More about side effects below).
The biologics are given by different methods. The nine we evaluate here are given by needle (Xeljanz, which was not included in our analysis, is a tablet taken by mouth). Some of them have to be administered slowly into a vein in your arm (intravenously), while others must be injected under the skin (subcutaneously), like insulin injections for diabetes. How often you will have to take a biologic depends on which drug you have been prescribed. You should discuss with your doctor whether or not you feel comfortable injecting yourself or whether you prefer an intravenous infusion at your doctor's office. Table 2, below, summarizes how individual biologics are given and how often.
| Generic Name | Brand Name | Administration | Must be repeated |
| Abatacept | Orencia | Intravenous infusion or subcutaneous injection* | Intravenous - every 4 weeks Subcutaneous - weekly |
| Adalimumab | Humira | Subcutaneous injection | Every week or every other week |
| Anakinra | Kineret | Subcutaneous injection | Daily |
| Certolizumab | Cimzia | Subcutaneous injection | Every other week |
| Etanercept | Enbrel | Subcutaneous injection | Weekly |
| Golimumab | Simponi | Subcutaneous injection | Once a month |
| Infliximab | Remicade | Intravenous infusion | Every 4 to 8 weeks |
| Rituximab | Rituxan | Intravenous infusion | Two infusions separated by 2 weeks; repeat treatment after 24 weeks if new symptoms arise |
| Tocilizumab | Actemra | Intravenous infusion | Every 4 weeks |
* One intravenous dose initially is followed by regular subcutaneous injections.
Subcutaneous injection = injection under the skin.; Intravenous infusion = administered into a vein in arm.

If other rheumatoid arthritis medications, such as the conventional or nonbiologic DMARDs, have not provided you with sufficient relief from your rheumatoid arthritis symptoms, then you may want to consider trying a biologic. All of the biologics are very expensive. These drugs cannot cure rheumatoid arthritis, but they have been shown to help relieve symptoms in about 30 to 70 percent of people who use them.
The available evidence is not good enough to distinguish differences in the effectiveness of the biologics. So the main difference between these medications comes down to their safety profile or the side effects they cause. For example, anakinra (Kineret) has the highest rate of injection site reactions and is less commonly used to treat rheumatoid arthritis. Rituximab (Rituxan) causes more infusion reactions than the other biologics, and certolizumab (Cimzia) might have higher rates of serious infections.
That leaves six remaining biologics. There is more evidence overall on three—adalimumab (Humira), etancercept (Enbrel), and infliximab (Remicade). A large study—known as the DREAM study—used patient records to evaluate these medications in people who were not helped by taking conventional DMARDs. Humira and Enbrel appeared to be equally effective in treating rheumatoid arthritis. Also, similar numbers of people stopped taking each drug due to side effects, suggesting both drugs have similar side effect profiles.
The DREAM study also compared Humira to Remicade. The two drugs were similar in effectiveness, but Humira had a lower rate of people dropping out due to side effects. The DREAM study was not a randomized, controlled clinical trial, since it was based on patient records, so the results are not as robust as they would be if this had been a clinical trial.
Several additional studies suggested Enbrel is more effective than Remicade. An analysis that combined the results of many small trials of all the biologics also suggested that Enbrel is the most effective, but the results of these types of analyses are often not reliable.
| Generic Name | Brand Name | Response to Treatment1 | Discontinuation because of side effects2 | Comments / Special Notes |
| Abatacept | Orencia | 26% - 40% | 3% - 7% | Low rate of infusion reactions |
| Adalimumab | Humira | 24% - 97% | 5% - 9% | None |
| Anakinra | Kineret | 19% - 50% | Not reported | Highest rate of injection site reactions |
| Certolizumab | Cimzia | 24% - 41% | 1% - 7% | Highest rate of serious infections |
| Etanercept | Enbrel | 47% - 100% | 3% - 57% | None |
| Golimumab | Simponi | 16% - 40% | 2% - 6% | None |
| Infliximab | Remicade | 27% - 75% | 2% - 20% | Higher rate of infections than Orencia and Enbrel |
| Rituximab | Rituxan | 18% - 49% | 1% - 6% | Highest rate of infusion reactions3 |
| Tocilizumab | Actemra | 29% - 54% | 4% - 12% | None |
1. Response is defined as an at-least 50 percent improvement of rheumatoid arthritis symptoms. Based on multiple studies and combined analysis of studies, or from the drug's product label information. Figures are not meant to imply that drugs were necessarily compared to each other in a study with consistent design.
2. Average discontinuation rates due to adverse events seen in studies. Based on multiple studies and combined analysis of studies, or from the drug's product label information. Figures are not meant to imply that drugs were necessarily compared to each other in a study with consistent design.
3. 77 percent of people treated with rituximab had a reaction after the first infusion.
One study known as ATTEST found abatacept (Orencia) to be more effective after one year of treatment than infliximab (Remicade) in people who had not gotten adequate symptom relief from methotrexate (Rheumatrex, Trexall, and generic). Orencia also appears to have a lower rate of infections, serious infections, serious adverse events, and infusion reactions than Remicade. In addition, more people in the study discontinued treatment with Remicade. One problem with this study, however, is that the people taking Remicade were not allowed to increase their dose, which is often necessary in a real world setting.
There is no evidence comparing the two remaining biologics—golimumab (Simponi) and tocilizumab (Actemra). There are no trials that have compared them against each other and there are no studies that could be used to compare either of them against the other biologics.
Side effects are an important consideration with this group of biologics. In studies, people who took a biologic had a higher risk—13 percent versus 12 percent—of experiencing a serious life-threatening allergic reaction, infection, lymphoma, or other serious side effect than those who took a placebo. The serious or potentially life-threatening infections include bacterial infections, such as tuberculosis, pneumonia, or staph, and serious fungal infections. Minor side effects can also occur, but usually do not require stopping or changing drugs.
The mild side effects associated with these medications include: diarrhea, headache, injection-site reactions, nausea, respiratory infection, urinary tract infection
Serious side effects can include: allergic reactions, liver damage, lymphoma, serious infections.
All of the biologics carry warnings on their labeling about serious side effects, particularly serious infections.
You should not take two or more biologics in combination. Studies show that when two or more biologics are taken at the same time, there is a substantially higher rate of serious adverse events than taking one of the drugs alone. Specific combinations that have been shown to have more adverse events include Kineret with Enbrel, and Orencia with Enbrel.
Rituxan appears to have a higher potential for infusion reactions than other biologics. In addition, it has been linked to an increased risk of a serious viral infection of the brain. The infusion reactions can be severe and even fatal. Because of this, it should only be used as a second-line therapy if other biologics do not provide enough symptom relief.
Remicade has been shown to have a high rate of serious side effects, and is also not one of the top picks. One trial found that, compared to Orencia, Remicade had higher rates of serious adverse events (18.2 percent compared with 9.6 percent), and serious infections (8.5 percent compared with 1.9 percent).
Table 3, above, is a summary of each drug's effectiveness and the percentage of study participants who stopped taking each biologic due to its side effects. The table also contains comments on noteworthy issues associated with each drug.
The available evidence indicates that Orencia and Kineret have the lowest risk of serious side effects. However, Kineret, which is given as an injection under the skin every day, causes more redness, itching, rash, and pain at the injection site than the other biologics that are given in this way.
In addition to effectiveness and safety, choosing a biologic involves several other factors, including the frequency of use, how the drug is given, and the length of time the treatment is effective. Also, because of the significant cost of these drugs, how much your insurance will provide coverage and how much you will pay out-of-pocket, will all factor into deciding which biologic therapy may be best for your situation.
Taking into account the evidence for effectiveness and safety, as well as cost, if you need a biologic drug to treat your rheumatoid arthritis, we have chosen the following asConsumer Reports Best Buy Drugs:
■ Abatacept (Orencia)
■ Adalimumab (Humira)
■ Etanercept (Enbrel)
Studies show that these three medications are as effective as the other biologics for relieving rheumatoid arthritis symptoms, and they also may have lower rates of withdrawal due to adverse effects than some other biologics.
This information is based on an analysis of the clinical evidence on the effectiveness and safety of biologic therapies for rheumatoid arthritis done by the Drug Effectiveness Review Project (DERP). In this analysis, a total of 4,736 studies and research articles dealing with any use of biologic drugs were identified and screened. All were published between 1990 and 2011. As a supplement to the DERP report, we also reviewed additional analyses, including some done by the Cochrane Review, that were published in 2011 and 2012.
From these, the analysis focused on 163 studies involving the use of biologics to treat people with rheumatoid arthritis, which included 70 controlled clinical trials, 31 studies that performed an analysis of multiple other studies, 51 observational studies, and 11 studies of other design. An additional 255 articles were reviewed for general background information pertinent to biologic chemistry, biology, and clinical use.
Balancing the effects between benefit and harm is particularly challenging because there is a lack of long-term data on the safety of biologics from controlled trials. There are large registries of patients that are intended to address long-term safety, but they have had conflicting results. They have also focused on biologics vs. DMARDs rather than on comparing different biologics.

How Effective are Biologics?
For many people who have not responded to standard rheumatoid arthritis treatment (conventional DMARDs, for example), the biologics can be effective treatments. However, people's responses vary—some experience a vast improvement in their symptoms and function, while others may experience little or no improvement at all. It is important to note that the studies of biologics have involved people who had failed on other rheumatoid arthritis medications, so we strongly recommend trying conventional DMARDs and other medications first before going to a biologic.
The effectiveness and benefits of biologics are primarily assessed on three criteria:
■ People's response to treatment, often characterized by at least 50 percent improvement in rheumatoid arthritis symptoms on a rheumatoid arthritis rating scale.
■ Whether there is slowing of the progression of the disease and prevention of joint damage.
■ Whether there are improvements in people's quality of life and function.
Response to treatment is based on how people rate their pain, stiffness, and other symptoms. On average, between 25 and 50 percent of people who do not respond to conventional DMARDs and switch to a biologic can expect to experience at least a 50 percent improvement in their symptoms as compared to those who continue to take conventional DMARDs. Roughly 40 percent of people will fail to respond to any particular treatment, and will likely require a switch to another biologic. As we have previously noted, however, two biologics should never be taken at the same time, because this significantly increases the chance of adverse effects, but with little improvement in symptoms.
If you are on Remicade, you may require a dose adjustment after a few months of treatment. Many patients need to adjust their treatment to larger doses to maintain the response. Larger doses for all biologics increase the risk of side effects.
Longer and more extensive studies have been conducted on some of the biologics more than on others. Most trials of biologics are relatively short, lasting between three to 12 months, and only a handful have compared biologics directly to each other in terms of effectiveness and safety. The limited time frame does not allow an assessment of long-term response or safety in a chronic, progressive disease. As mentioned above, biologics cannot cure rheumatoid arthritis, but they may help slow the progression, alleviate the symptoms, and may prevent joint damage.
While television and magazine ads often tout the benefits of starting biologics early during the course of disease, studies in people with early rheumatoid arthritis have not shown any clear benefits of biologics over conventional DMARD treatment when starting treatment for the first time. People responded to both treatments equally well, but conventional DMARDs are vastly cheaper than biologics and should be the first line of treatment in people with newly diagnosed rheumatoid arthritis. Additionally, the bulk of evidence underlying the effectiveness and safety of the biologics is based on studies involving people in whom conventional DMARDs were ineffective. In other words, these drugs should only be used if you do not get adequate symptom relief from other therapies, including exercise, over-the-counter and prescription pain relieving drugs, and conventional DMARDs, like methotrexate (Rheumatrex, Trexall, and generic).
How Safe are the Biologics?
As discussed earlier, studies show that about 13 percent of people who take a biologic experience serious or life-threatening side effects, compared with about 12 percent who receive a placebo. Because biologics target the defense system of your body, minor infections, such as respiratory infections or urinary tract infections, are common. In addition, nausea and joint pain can also occur. Depending on the drug, side effects related to drug administration are common. For biologics that are injected subcutaneously (abatacept, adalimumab, anakinra, certolizumab, etanercept, and golimumab), injection site reactions, such as rash, itching, and pain, are common. Anakinra appears to cause more injection-site reactions than the other biologics.
Reactions to the intravenous infusion of a biologic (abatacept, infliximab, rituximab, and tocilizumab) are also common. Such infusion reactions include dizziness, chills, itching, headaches, and fever. In about 1 percent of patients, infusion reactions can be severe and can mimic a severe allergic reaction or lead to convulsions. Deaths have also been reported following infusions of biologics. Rituximab appears to have a higher risk for such reactions than other biologic drugs.
Long-term risks of biologics are also a concern. These may include severe infections, particularly tuberculosis and fungal infections. Other infections have been reported, and some have resulted in death. All biologics carry on their labeling warnings about the increased risk of infections.
Biologics are also associated with an increased risk of skin cancers. It was previously thought that the biologics might also increase the risk of cancers involving lymph nodes and bone marrow, but data from multiple studies has not shown this to be the case. However, the FDA continues to warn about this risk (the most recent update was issued in April 2011), and the package insert of biologics still carries a black box warning about lymphoma.
Other adverse effects include worsening or triggering congestive heart failure, liver damage, and neurologic disorders. Long-term adverse effects have yet to be thoroughly studied and identified.
To reduce the risk of side effects, let your doctor know if you have:
■ chronic obstructive pulmonary disease (COPD)
■ diabetes
■ an infection or history of infections
■ tuberculosis or a positive skin test for tuberculosis
■ viral hepatitis
Also notify your doctor if you have been around an individual with chicken pox, shingles, or tuberculosis, or if you are scheduled to receive a vaccine or have surgery.
The risk of biologics to unborn babies is unknown. Women of child-bearing age should use contraception while on biologics. If you are planning to become pregnant, talk with your doctor about when to stop using contraception and biologics. The labeling of biologics advises these medications not be used by pregnant women unless necessary.
Drug Interactions
Biologics are often prescribed together with other medications, such as methotrexate, pain medications, or corticosteroids, and do not seem to interact with most drugs. But it's important to note that there is little research on how the biologics interact with other drugs. Biologics, however, should never be taken together with other biologics, as this can increase the risk of severe adverse effects.
Because biologics affect your immune system, it is recommended that you should not be immunized with ‘live' vaccines, such as the yellow fever vaccine, while you are on biologic therapy. In certain situations, however, a live vaccine may be necessary (for example, rubella immunization in women of childbearing age). You should discuss the possible risks and benefits of immunizations with your doctor. Other vaccines, such as flu vaccines (but not the nasal flu vaccine, FluMist, which contains live virus), are safe, and can be administered with biologic medications. But read the package insert of the biologic you are taking, and also discuss with your doctor any vaccines you plan to take.
Age, race, and gender differences
People older than 65 and various ethnic groups have been under-represented in most studies of biologics. Still, the existing evidence does not indicate that any biologic is more or less effective in older patients, people of any particular race or gender, or in patients who have other diseases.
| Considerations | Details |
| Effectiveness | 25 to 50 percent of people who take biologics can expect to experience at least a 50 percent improvement in the number of swollen or tender joints. |
| Safety | In studies, about 13 percent of people who took a biologic experienced serious or life-threatening side effects (but many people, about 12 percent, who received a placebo also had serious side effects). Minor side effects, such as abdominal pain, nausea, and injection site reactions, can also occur—but usually do not require—stopping or changing drugs. All biologics carry risk of serious side effects, including infections. Rituximab (Rituxan) and anakinra (Kineret) have higher rates of injection and infusion site reactions, and certolizumab (Cimzia) and infliximab (Remicade) have a higher risk of infections. |
| Cost | Can cost up to several thousand dollars per month, if paying out-of-pocket. |
| Insurance coverage | Find out if your chosen treatment will be covered by your insurance. The range of coverage, co-pays, and other expenses will likely ultimately determine your biologic choice. |
| Availability of product/staff/facilities to administer | Your health care providers might be more familiar with specific biologics, some products might be more available, and facilities to administer some products might be more easily accessible. |
| Need to switch (Failure with another therapy) | Roughly 40 percent of people are not helped by the first treatment they receive, and might have to be switched to another biologic. How you respond to a first biologic will determine decisions about how to choose the second or third biologic. |
| Frequency of administration | These drugs are given with varying frequencies, such as daily, weekly, monthly, or bimonthly. This may affect your choice of biologic. |
| Route of administration | Self injection, physician injection or intravenous infusion (See Table 2, above). |
| Harm related to route of administration | Infusion reactions and injection site reactions can be common, but most are mild (headache, dizziness, nausea, itching, chills, fever). |

Our evaluation is based in part on an independent scientific review of the studies and research literature on biologic therapies conducted by a team of physicians and researchers at the Oregon Health & Science University Evidence-Based Practice Center. This analysis reviewed more than 163 studies, that included 70 controlled clinical trials, 31 studies that performed a cross-cutting analysis of multiple other studies, 51 observational studies, and 11 studies of other design. This effort was conducted as part of the Drug Effectiveness Review Project, or DERP. DERP is a first-of-its-kind, multistate initiative created to evaluate the comparative effectiveness and safety of hundreds of prescription drugs.
A synopsis of DERP's analysis of the biologic drugs forms the basis for this report. A consultant to Consumer Reports Best Buy Drugs is also a member of the Oregon-based research team, which has no financial interest in any pharmaceutical company or product. The full DERP review of the biologic drugs to treat rheumatoid arthritis is available at https://derp.ohsu.edu/about/final-documentdisplay.cfm. (Note that this is a long and technical document written for physicians and other medical researchers.)
The monthly costs we cite were obtained from Source Healthcare Analytics, Inc., a health-care information company that tracks the sales of prescription drugs in the U.S. Prices for a drug can vary quite widely. All the prices in this report are national averages based on sales in retail stores only. They reflect the cash price paid for a month's supply of each drug in December 2012.
Consumer Reports selected the Best Buy Drugs using the following criteria. The drug had to:
■ Be approved by the FDA to treat rheumatoid arthritis.
■ Be as effective as or more effective than other biologics when prescribed appropriately according to FDA guidelines based on published randomized controlled trials.
■ Have a safety record equal to or better than other biologics medicines when prescribed appropriately.
The Consumers Reports Best Buy Drugs methodology is described in more detail in the Methods section at www.CRBestBuyDrugs.org.
Alonso-Ruiz, A., J. I. Pijoan, et al. (2008). "Tumor necrosis factor alpha drugs in rheumatoid arthritis: systematic review and metaanalysis of efficacy and safety." BMC Musculoskelet Disord 9: 52.
Askling, J., C. M. Fored, et al. (2007). "Time-dependent increase in risk of hospitalisation with infection among Swedish RA patients treated with TNF antagonists." Annals of the Rheumatic Diseases 66(10): 1339-1344.
Bathon, J. M., R. W. Martin, et al. (2000). "A comparison of etanercept and methotrexate in patients with early rheumatoid arthritis." N Engl J Med 343(22): 1586-93.
Blumenauer, B., A. Burls, et al. (2002). "Infliximab for the treatment of rheumatoid arthritis." The Cochrane Database of Systematic Reviews(3).
Bongartz, T., A. J. Sutton, et al. (2006). "Anti-TNF Antibody Therapy in Rheumatoid Arthritis and the Risk of Serious Infections and Malignancies: Systematic Review and Meta-analysis of Rare Harmful Effects in Randomized Controlled Trials." JAMA 295(19): 2275-2285.
Brassard, P., A. Kezouh, et al. (2006). "Antirheumatic drugs and the risk of tuberculosis." Clin Infect Dis 43(6): 717-22.
Breedveld, F. C., M. H. Weisman, et al. (2006). "The PREMIER study: A multicenter, randomized, double-blind clinical trial of combination therapy with adalimumab plus methotrexate versus methotrexate alone or adalimumab alone in patients with early, aggressive rheumatoid arthritis who had not had previous methotrexate treatment." Arthritis Rheum 54(1): 26-37.
Clark, W., P. Jobanputra, et al. (2004). "The clinical and cost-effectiveness of anakinra for the treatment of rheumatoid arthritis in adults: a systematic review and economic analysis." Health Technol Assess 8(18): iii-iv, ix-x, 1-105.
Cohen, S. B., P. Emery, et al. (2006). "Rituximab for rheumatoid arthritis refractory to anti-tumor necrosis factor therapy: Results of a multicenter, randomized, double-blind, placebo-controlled, phase III trial evaluating primary efficacy and safety at twenty-four weeks." Arthritis and Rheumatism 54(9): 2793-2806.
Emery, P., R. Fleischmann, et al. (2006). "The efficacy and safety of rituximab in patients with active rheumatoid arthritis despite methotrexate treatment: Results of a phase IIB randomized, double-blind, placebo-controlled, dose-ranging trial." Arthritis Rheum 54(5): 1390-400.
Gartlehner, G., R. A. Hansen, et al. (2006). "The comparative efficacy and safety of biologics for the treatment of rheumatoid arthritis: a systematic review and metaanalysis." J Rheumatol 33(12): 2398-408.
Geborek, P., M. Crnkic, et al. (2002). "Etanercept, infliximab, and leflunomide in established rheumatoid arthritis: clinical experience using a structured follow up programme in southern Sweden." Ann Rheum Dis 61(9): 793-8.
Genovese, M. C., S. Cohen, et al. (2004). "Combination therapy with etanercept and anakinra in the treatment of patients with rheumatoid arthritis who have been treated unsuccessfully with methotrexate." Arthritis Rheum 50(5): 1412-9.
Hochberg, M. C., J. K. Tracy, et al. (2003). "Comparison of the efficacy of the tumour necrosis factor alpha blocking agents adalimumab, etanercept, and infliximab when added to methotrexate in patients with active rheumatoid arthritis." Ann Rheum Dis 62 Suppl 2: ii13-6.
Keystone, E., P. Emery, et al. (2009). "Rituximab inhibits structural joint damage in patients with rheumatoid arthritis with an inadequate response to tumour necrosis factor inhibitor therapies." Ann Rheum Dis 68(2): 216-21.
Kievit, W., E. M. Adang, et al. (2008). "The effectiveness and medication costs of three antitumour necrosis factor alpha agents in the treatment of rheumatoid arthritis from prospective clinical practice data." Ann Rheum Dis 67(9): 1229-34.
Kristensen, L. E., T. Saxne, et al. (2006). "The LUNDEX, a new index of drug efficacy in clinical practice: results of a five-year observational study of treatment with infliximab and etanercept among rheumatoid arthritis patients in southern Sweden." Arthritis Rheum 54(2): 600-6.
Navarro Sarabia, F., R. Ariza Ariza, et al. (2006). "Adalimumab for treating rheumatoid arthritis (Brief record)." Journal of Rheumatology(6): 1075; 1081-1075; 1081.
Schiff, M., M. Keiserman, et al. (2008). "Efficacy and safety of abatacept or infliximab vs placebo in ATTEST: a phase III, multi-centre, randomised, double-blind, placebo-controlled study in patients with rheumatoid arthritis and an inadequate response to methotrexate." Ann Rheum Dis 67(8): 1096-103.
Setoguchi, S., S. Schneeweiss, et al. (2008). "Tumor necrosis factor-(alpha) antagonist use and heart failure in elderly patients with rheumatoid arthritis." American Heart Journal 156(2): 336-341.
Singh J.A., R. Christensen R, et al. (2009). "Biologics for rheumatoid arthritis: an overview of Cochrane reviews." The Cochrane Database of Systematic Reviews(4).
Singh JA, Beg S, et al. (2010). Tocilizumab for rheumatoid arthritis. Cochrane Database of Systematic Reviews 2010, Issue 7. Art. No.: CD008331. DOI: 10.1002/14651858.CD008331.pub2.
Singh JA, Furst DE, et al. (2012) 2012 Update of the 2008 American College of Rheumatology Recommendations for the Use of Disease-Modifying Antirheumatic Drugs and Biologic Agents in the Treatment of Rheumatoid Arthritis. Arthritis Care & Research, Vol 64, No. 5, May 2012, pp 625-639.
Singh JA, Noorbaloochi S, et al. (2010). Golimumab for rheumatoid arthritis. Cochrane Database of Systematic Reviews 2010, Issue 1. Art. No.: CD008341. DOI: 10.1002/14651858.CD008341.
Singh JA, Wells GA, et al. (2011). Adverse effects of biologics: a network meta-analysis and Cochrane overview. Cochrane Database of Systematic Reviews 2011, Issue 2. Art. No.: CD008794. DOI: 10.1002/14651858.CD008794.pub2.
Thaler KJ, Gartlehner G, et al. (2012) Drug class review: Targeted immune modulator. Final update 3 report. Prepared by the RTI-UNC Evidence-based Practice Center for the Drug Effectiveness Review Project. Oregon Health & Science University. Portland, OR. 2012. Available at: https://derp.ohsu.edu/about/final-document-display.cfm.
Wailoo, A., A. Brennan, et al. (2006). "Modeling the cost effectiveness of etanercept, adalimumab and anakinra compared to infliximab in the treatment of patients with rheumatoid arthritis in the Medicare program. AHRQ Technology Assessment Program."
Weaver, A. L., R. L. Lautzenheiser, et al. (2006). "Real-world effectiveness of select biologic and DMARD monotherapy and combination therapy in the treatment of rheumatoid arthritis: results from the RADIUS observational registry." Curr Med Res Opin 22(1): 185-98.
Weinblatt, M., M. Schiff, et al. (2007). "Selective costimulation modulation using abatacept in patients with active rheumatoid arthritis while receiving etanercept: a randomised clinical trial." Ann Rheum Dis 66(2): 228-34.
Wolfe, F. and K. Michaud (2007). "Biologic treatment of rheumatoid arthritis and the risk of malignancy: Analyses from a large US observational study." Arthritis and Rheumatism 56(9): 2886-2895.
These materials are made possible by a grant from the state Attorney General Consumer and Prescriber Education Grant Program, which is funded by the multi-state settlement of consumer-fraud claims regarding the marketing of the prescription drug Neurontin (gabapentin).
 WASHING MACHINE REVIEWS
WASHING MACHINE REVIEWS GENERATOR REVIEWS
GENERATOR REVIEWS
 Build & Buy Car Buying Service
Build & Buy Car Buying Service
Save thousands off MSRP with upfront dealer pricing information and a transparent car buying experience.
 Get Ratings on the go and compare
Get Ratings on the go and compare
while you shop