Last August, Martin Shkreli, then the CEO of Turing Pharmaceuticals, did something considered so reprehensible that he was dubbed "the most hated man in America." What caused the outrage? He increased the price of a little-known but important drug called Daraprim from $13.50 to $750 per pill. Daraprim is the best treatment for toxoplasmosis, an infection to which those with HIV/AIDs or cancer are susceptible.
The story went viral, and calls came from around the country, including from U.S. Rep. Elijah Cummings, D-Md., to stop drug entrepreneurs from gouging consumers for pure profit. Overnight, Shkreli became the poster child of pharmaceutical greed. And yet raising the price of a drug by that much is 100 percent legal.
What makes the case of Daraprim so important is that it brought a serious—and growing—healthcare problem out into the open: America spends a tremendous amount of money for prescription drugs—$424 billion last year alone before discounts, according to a new report by IMS Institute for Healthcare Informatics, a firm that tracks the pharmaceutical industry. And that number is rising fast with no sign of slowing down. What's more, there are few regulations that shield consumers from the Martin Shkrelis of the world, or from drug companies that decide to raise prices to astronomical levels.

The Rampant Rise of Drug Prices
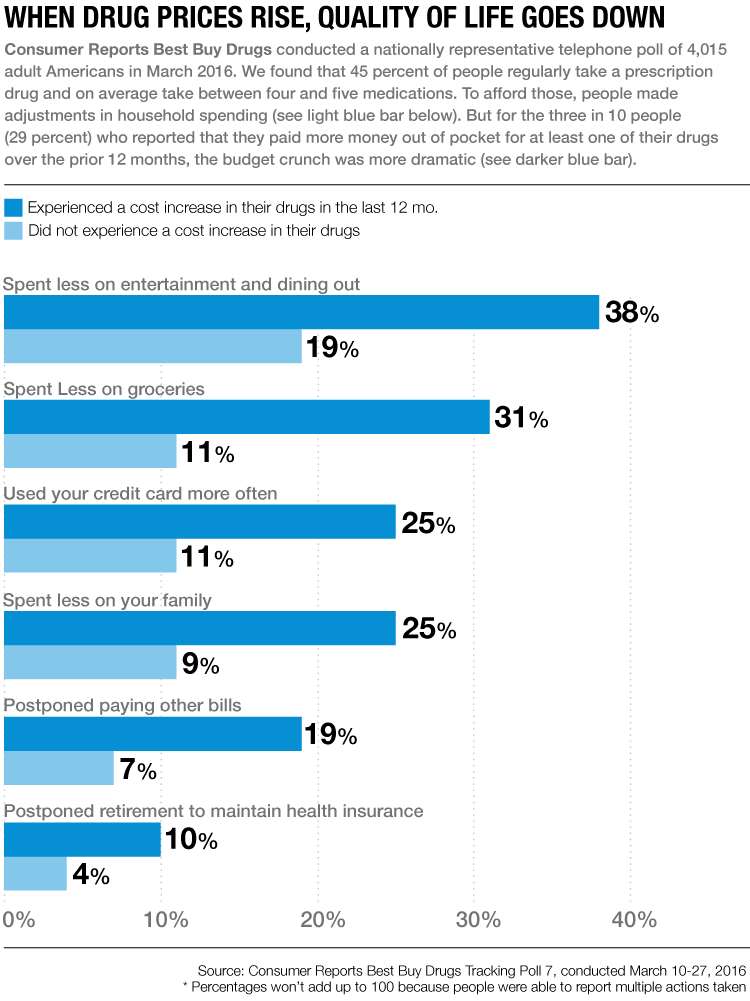
The practice of raising drug prices on new—and old—medications is common and widespread. From a nationally representative telephone poll conducted by Consumer Reports Best Buy Drugs in March, we learned that three in 10 Americans (about 32 million people) were hit with price hikes within the previous 12 months, costing them an average of $63 more for a drug they routinely take—and a few paid $500 or more. We also found price increases on everything from longtime generics used to treat common conditions such as diabetes, high blood pressure, and high cholesterol to new treatments for diseases such as hepatitis C. Our poll shows that when people were hit with higher drug costs, they were more likely to take unhealthy measures such as skipping doctor appointments, tests, or procedures, or not filling their prescriptions or taking them as directed.
Take the case of Marlene Condon, a nature writer living in Crozet, Va. Two years ago she paid about $32 for 180 tablets of hydroxychloroquine (a generic available for almost two decades) to treat her rheumatoid arthritis. When the drug's price more than doubled to $75, Condon says she was annoyed but paid the bill anyway. Then, last September, the price of her drug skyrocketed, costing her $500 out of pocket. Condon panicked and did what thousands of Americans do under those circumstances: She stopped taking the drug. Her arthritis pain grew much worse. Walking and doing simple household chores such as washing the dishes became almost impossible.
The Way To Save On Your Prescription Drugs: Speak Up
The Forces of Profit
Our analysis suggests that high prices for generic and brand-name drugs stem in part from a battle over profit between mammoth industries—big pharma and insurance companies—with consumers caught in the middle. On the one hand, pharmaceutical companies blame insurance companies for passing along high costs to consumers. And insurance companies point to very high-priced drugs for which there are few or no alternatives, which ultimately affects how much insurance coverage people receive and how much they must pay out of their pockets.
"Even as more patients have health insurance coverage, many more are facing high pharmacy deductibles and rising out-of-pocket costs, and other barriers to care, putting their ability to stay on needed therapy at risk," says Holly Campbell, a representative at PhRMA, an industry association that represents pharmaceutical manufacturers.
"If there's one treatment and there's no alternative and no competition, then that's where the challenge is," says Matt Eyles, executive vice president of policy and regulatory affairs at America's Health Insurance Plans (AHIP), a national trade organization for the insurance industry.
The first step in attempting to correct prices for the consumer good is to understand and acknowledge how we got to this moment. Here, a closer look at the reasons drug costs are ballooning:
Reason 1: Drug Companies Can Charge Whatever Price They Want
Nothing protected Condon from the price increases she experienced. That's because for Medicare and commercial health plans, no government body—including the Federal Trade Commission, the Food and Drug Administration, and the Centers for Medicare & Medicaid Services—has rules or laws that dictate or restrict the price a pharmaceutical company can set for a drug. And in most cases, there's nothing that restricts how much a company can raise that price. Here's an example: Last year, on the same day that Valeant Pharmaceuticals purchased the rights to lifesaving heart drug Isuprel (isoproterenol) and blood pressure medication Nitropress (nitroprusside), the company jacked up the prices. A single dose of Isuprel rose from $180 to $1,472, and Nitropress went from $215 to $1,346. The company also purchased Cuprimine (penicillamine)—a drug used to treat Wilson's disease, a rare genetic disorder—and upped its price from $8.88 to $262 per capsule. In all three cases, the drugs had no generic equivalents available, so Valeant was able to corner the market with a built-in base of customers.
"Valeant raised the price of these drugs after an analysis of their actual value," says company representative Laurie Little.
These huge increases have drawn congressional attention because the U.S. government is the largest purchaser of drugs in the country for programs including Medicare and Medicaid, as well as for veterans and the military. Spending more money on drugs because of price increases can mean more taxpayer dollars are used than originally budgeted—something Congress must manage. Last fall, Sens. Susan Collins, R-Maine, and Claire McCaskill, D-Mo., launched a large-scale investigation into sudden and aggressive price increases by four drugmakers, including Turing and Valeant, requesting that the companies turn over documentation to justify the hikes. And earlier this year, Rep. Cummings held a similar congressional hearing, releasing reams of internal memos to the public that detailed the profit goals that companies like Turing were trying to reach by setting the price hikes.
Stephen Lederer, a spokesman for Turing, said the company's pricing for Daraprim "reflected its clinical value." He notes that the company also funded access programs so that a person's insurance co-pays would amount to $10 and provided the drug free to certain disadvantaged patients.
Price manipulations aren't limited to small pharmaceutical firms: Major firms raked in an additional $25.6 billion (gross) in 2015 simply by raising prices on their brand-name drugs, according to a recent report by the IMS. The firm estimates that figure to grow to $155 billion over the next five years.
How do drug companies explain high prices and price hikes? Says Campbell on behalf of PhRMA: "There are many factors that go into a price of a medicine." Those include the drug's "clinical merits"—how well it works, Campbell notes, and whether it reduces other healthcare costs, for example, such as reducing the need for surgery or other types of medical care.
More on High Drug Prices
But other considerations may factor into how a drug's value is determined. For example, in the U.K., a centralized advisory board calculates the value of a medication by taking into account a drug's efficacy, safety, and total benefits to the healthcare system and to society at large. In the U.S., no such central advisory board exists; we effectively leave it up to industry to make that determination instead.
PhRMA's Campbell adds that the price a drug company sets also takes into account expenses involved in research and development. Plus, "revenue from commercially successful medicines is reinvested in research for the next generation of treatments." She points to data from a recent PhRMA survey of member companies that found that companies invested $58.8 billion on research and development in 2015, up 10.3 percent from the prior year.
But American taxpayers already shoulder a substantial burden of those costs. About 38 percent of all basic science research is paid for with tax money through federal and state governments, according to a 2015 study published in the Journal of the American Medical Association.
Moreover, drug companies may spend up to twice as much or more on marketing and promoting their products—including advertising—as they do on research and development. That's according to a new analysis published in the Annals of Internal Medicine in March 2016. Says Wayne Riley, M.D., immediate past president of the American College of Physicians (ACP), one of the largest physician groups in the U.S. and the organization that did the review: "Pharmaceutical companies may price drugs at will, and in truth, it's not clear what that price is based on."
In fact, it would seem that the spending drug companies need to recoup with higher prices is at least partly due to how much is spent on direct-to-consumer advertising. Our review of the 2015 annual reports of 10 of the world's largest drug companies revealed that all spent more on marketing and administration costs than research and development. Ideally, a drug company will spend a substantial portion of its revenue in R&D seeking new discoveries—finding new medical treatments and cures. We found that drug company behemoths Johnson & Johnson and Pfizer spent about 13 percent and 16 percent on R&D, respectively. At the same time, both companies spent about 30 percent of revenue on selling, marketing, and administrative expenses.
The drug industry doesn't play by the same rules as any other market, where exorbitant prices dissuade customers, says Kevin Riggs, M.D., a researcher at the Johns Hopkins University, where he focuses on healthcare costs. "A drug company can increase the price of a product many times over, and people will still buy it because they need it," he says. "At the end of the day, they largely charge whatever the market will bear—and with lifesaving medication, that's a lot."
Reason 2: Insurance Companies Are Also Charging You More
Insurance companies exist, in theory, to protect people from unexpected high costs of healthcare. You pay a monthly premium that goes into large "pool." The idea is that should you need to draw from that pool to pay for a healthcare expense, it's there for you. In the case of drugs, insurance companies often work with firms called pharmacy benefit managers, or PBMs, that further pool consumers together to negotiate large-volume discounts from drug companies. The idea is that those discounts will ultimately save you money.
The only way left for insurers to provide coverage for a drug but maintain their profit margins is to reduce how much insurance coverage—and thus protection from high prices—they offer to a consumer. That can happen in at least one of four ways: by raising your deductible; by increasing monthly premiums; by increasing your co-pay by putting drugs into more expensive "tiers"; or by making you pay "co-insurance," where you pay a percentage of the medication's cost; usually one-third or more.
"The dramatic increase in prescription drug costs is definitely contributing to a move" to higher insurance deductibles and greater cost sharing with consumers, says Eyles from AHIP, the insurance industry trade organization.
Ten years ago, less than 10 percent of employees with health insurance were enrolled in a plan with a deductible of $1,000 or more. Today, almost half (46 percent) of Americans have those plans, according to research by the Kaiser Family Foundation, a nonprofit organization focused on national health concerns.
Eyles says that insurers have limited leverage with drugmakers, especially when it comes to new and expensive drugs. "There's not a lot we can do other than say we won't cover it, and that's an extreme most plans want to avoid."
But that's exactly what has happened. For its 2016 formulary—the list of drugs covered—Express Scripts, the largest PBM in the U.S., dropped coverage of 80 drugs, including insulins such as Novolin and NovoLog for people with type 1 diabetes, and instead offering coverage for Humulin and Humalog. The company noted in its announcement about the change that it "only exclude[s] medications from our formulary when clinically equivalent alternatives are already covered on our formulary, and only then when those exclusions would result in significant cost savings for our clients and patients."
Reason 3: Old Drugs Are Reformulated as Costly ‘New' Drugs
Reinventing old medications is a tactic called evergreening—where companies change or tweak the formula of a drug by, say, combining two older drugs to form a "new" pill. Or they create an extended-release version, or change the delivery method—for example, instead of a tablet or an injectable, the new version is inhaled. When that happens, the federal government may grant the drug company a new patent, which could be worth up to 20 years of protection for its drug, meaning it may not have any generic drug competitors. That can translate to greater revenue for a pharmaceutical company and higher costs for the consumer.
One example is the diabetes drug insulin. The drug is almost 100 years old, and yet no generic version is available in the U.S. That's because drug companies keep changing its formulation and getting new patents for it. Thomas Woodard, 73, of Greensboro, N.C., takes a newer form of insulin called Toujeo. Instead of taking multiple daily injections, he gives himself a single daily injection from a pen that lasts about a week. (To be sure, injecting less frequently is more convenient.) Woodard pays about $85 per month for the drug, but there's a problem: When Woodard fills his prescription, the pharmacy and his insurance company will permit him only three pens, which don't entirely cover him for the month, and he can't afford another set of three pens. (They come in a box of three, and pharmacies can't break them up.) So he deals with it another way. "I get to the end of the month, and I just cut back on the number of units I take," Woodard says. That's not a good idea for a person with diabetes like Woodard, whose blood glucose level needs to remain fairly consistent. "Drug companies keep coming out with new insulins, which work better, but the price keeps going up," he says.*
Last year 30 products that were reformulations of old drugs hit the market, according to another recent report by the IMS. Says George Slover, senior policy counsel for Consumers Union, the advocacy arm of Consumer Reports: "Evergreening keeps drug prices high for consumers because it makes it harder for lower-cost generic alternatives to enter the market and give consumers a choice."
Reason 4: Generic Drug Shortages Can Trigger Massive Price Increases
Marlene Condon's experience with her medication's skyrocketing price is not an isolated event. Overall, prices of generics increased by almost 9 percent between November 2013 and November 2014, according to a 2015 report by Elsevier, a company that supplies information on drug pricing. Some prices remained stable or even dropped. But the cost of certain drugs went up—way up—when they should have stayed the same or even gone down.
"It's those huge price hikes in everyday drugs that are having the greatest impact on consumers," says Riley of the ACP. "Patients who have been taking generics for years are suddenly finding that their medication is unaffordable." In Marlene Condon's case, it's clear what made her generic arthritis drug, hydroxychloroquine, so expensive. First, some background: At least six companies are approved by the FDA to create generic copies of the drug Condon takes, including three of the biggest in the U.S.: Mylan, Sandoz, and Teva. In theory, having so many companies that make the same drug should increase competition and bring the price down. And that's exactly what happened for more than two decades.
But in recent years, several companies have stopped making older generic drugs such as hydroxychloroquine altogether because they said they couldn't make enough profit selling them. For example, Teva, the largest generic drugmaker, told us it stopped making the arthritis drug in 2012 because of "profitability challenges." Another company, West-Ward, ceased production of the drug in 2014.
When fewer companies make a drug, a new problem is created: If there are any hiccups with getting the drug's "raw" ingredients, it can affect the entire supply in the U.S. That's what happened with hydroxychloroquine, according to a representative from Sandoz, a pharmaceutical firm still making the drug. In 2014, a company that supplies the raw ingredient for the drug failed an FDA inspection and temporarily stopped making it—and soon there was a shortage. The two drugmakers that were able to still get the raw material then upped the price.
Condon's arthritis drug is still expensive, and now she finds discount drug coupons online that cut the cost to less than $300. But it's still a hardship.
What can protect us from sudden price hikes on old drugs? Apparently not the FDA. An agency spokesman, Christopher Kelly, told us the "FDA doesn't have a way to control what a company ultimately decides to charge under our present authorities." Kelly notes that the FDA pays particular attention to new generic drug applications from companies that would prevent shortages of medically necessary drugs. But "the pricing and decisions that companies make regarding pricing is an area currently outside FDA purview, and we have no enforcement capability in this area," Kelly notes.

Reason 5: Specialty Drugs Are Costing All of Us
The rise of super-expensive, so-called specialty drugs is a new threat. Examples include the hepatitis C medications Sovaldi ($84,000 for a 12-week course of treatment) and Harvoni (up to $95,000) that usually target small groups of patients with less common conditions. But their astronomical prices are driving up overall costs for the healthcare system.
Currently, specialty drugs account for less than 1 percent of prescriptions in the U.S. but represent about one-third of total drug spending by consumers, employers, and the government, which all purchase medications, according to a recent report by the Congressional Research Service. And as drug companies invest heavily in those highly profitable products, the IMS estimates that by 2020 very expensive drugs are likely to constitute an even bigger chunk of drug spending.
More than half of the 56 medications approved by the FDA in 2015 were specialty drugs. And more than 900 biologic drugs are currently under development, according to PhRMA. "We're all excited about these new technologies, but it's not at all clear how we as a society are going to pay for it," says Kevin Schulman, M.D., a professor of medicine and business administration at Duke University, where he is also director of the Center for Clinical and Genetic Economics and an associate director of the Duke Clinical Research Institute.
One thing is clear: Consumers' costs will rise. Most Medicare prescription plans require patients to pay one-third or more of the costs of specialty drugs. And consumers still face higher insurance premiums and deductibles, says Eyles of AHIP. "The dramatic growth in this part of the marketplace is unsustainable," he says. "Health plans just can't absorb those costs indefinitely without making adjustments to premiums and benefits."
Unfortunately, we can't always count on competition among drugmakers to drive down prices, says Riggs from Johns Hopkins. Many specialty drugs are biologics, medications that start out as a living organism derived from animals or humans, or from microorganisms, such as bacteria or yeast. That makes them much more difficult to copy than conventional drugs.
To date, the FDA has approved only two "biosimilar" drugs, essentially versions of already existing biologics. Even as those drugs trickle onto the market, Riggs says he's skeptical that biosimilar drugs would substantially lower prices; estimates predict price reductions between 20 and 40 percent, compared with about 80 percent for traditional generics.
What the Government Can Do
Consumers are looking to the government to take action to control drug prices. In our CR Best Buy Drugs poll, 77 percent of people taking a medication said the government should allow more generics onto the market sooner; 74 percent want the government to pressure drug companies to charge less. Seventy-nine percent say insurers should pressure pharmaceutical companies to lower drug prices; 81 percent said consumers should do the same.
More specific steps that could help control costs include asking the government to:
- Set a limit on out-of-pocket costs. That would ensure that consumers have some protection against very high costs or sudden large spikes in prices. For example, last year California enacted a law so that a consumer won't pay more than $250 for a single prescription drug per month, or $500 for certain high-deductible plans.
- Approve more generic versions of common drugs. Currently, 4,300 generic drug applications await an FDA decision. The agency says it's working to review new applications within 15 months.
- Allow limited importation of drugs from legitimate Canadian and European sources, which currently is illegal under U.S. law. The ability to import drugs from countries that have a regulatory system similar to that of the U.S. could alleviate shortages or moderate prices.
- Use government's existing "march-in" rights. It works like this: If there is a problem with the public's access to a drug (a supply shortage or an exorbitant price), and if a drug was developed using taxpayer money, the Department of Health and Human Services has the right to force the company to allow another manufacturer to make generic versions that are cheaper for the consumer.
What Drug Companies Can Do
The most obvious help pharmaceutical makers can provide is to charge less—or at least slow the pace of price increases. There is a precedent: Rising drug prices in the 1990s led to public outcry and congressional hearings. And fearing price controls, nine drug companies, led by Merck, made a pledge to keep price increases at or below increases in inflation.
"Pharma has a right to make a profit," says Riley of the ACP, but it also has a "moral obligation" to be transparent about its pricing because it benefits greatly from government-funded research. "The American taxpayer has been providing the venture capital to fund their products," he says. "The public deserves to realize a return on that investment in the form of medications they can afford." But pharmaceutical industry representatives think the focus on price alone is misguided and threatens "to squander our opportunity to usher in the next wave of medical progress," says Campbell at PhRMA.
States are starting to fight back. This past June, Vermont passed the first legislation in the U.S. that requires drug companies to justify high costs and price increases, and to calculate the financial effect on insurance premiums with a select set of drugs. California is currently considering a similar bill.

What Consumers Can Do
Although much of drug pricing is out of consumers' hands, consider these tips to find the best deals at the pharmacy:
- Talk to your doctor about the cost of the drug she is prescribing. For less expensive alternatives, ask about generics, which can cost up to 90 percent less. Your doctor might consider "therapeutic substitution"—a different drug that works as well. If your insurance drops or reduces coverage of a drug, your doctor can also help by appealing to your insurance company for an exception to cover the drug anyway. The administrative process for filing the exception is different with each insurance company and can take a few weeks before a decision is made.
- Shop around and negotiate. Consumer Reports' secret shoppers have found that retail drug prices can vary widely, even within the same ZIP code. Our shoppers also found that asking, "Is this your lowest price?" could get you further discounts.
- Check online. If you pay out of pocket, check GoodRx to learn a drug's "fair price." You can also fill a prescription with a low-cost online pharmacy based in the U.S., such as HealthWarehouse.com. Be careful of fraudulent websites: Use only an online retailer that operates within the U.S. and displays the VIPPS symbol to show that it's a Verified Internet Pharmacy Practice Site.
- Choose a plan that covers the medications you need. Compare plans during your open-enrollment period because coverage may change from year to year. Keep in mind that high-deductible plans have lower premiums but require you to pay a larger chunk of your drug costs.
Consumer Reports Is Working to Lower Drug Costs
You are outraged by rising drug costs, and we've listened. Because we do not accept money from the pharmaceutical industry, we can call it like it is. If a drug is too risky or a poor value, we are not afraid to say so. We want your voice to be heard by industry and government. We are advocating for a range of evidence-based solutions for lowering consumers' out-of-pocket costs, ensuring access to essential medicines, and getting better value for our country's prescription-drug spending—without sacrificing safety or effectiveness. See ConsumerReports.org/drugprices for more.
Editor's Note: This article also appeared in the August 2016 issue of Consumer Reports magazine.
Funding for the preparation of this article was provided in part by the Atlantic Philanthropies and by a grant from the state Attorney General Consumer and Prescriber Education Grant Program, which is funded by the multistate settlement of consumerfraud claims regarding the marketing of the prescription drug Neurontin (gabapentin).
*Clarification, July 29, 2016: An earlier version of this article indicated that Woodard's injection lasts about a week. He gives himself a daily injection from a pen that lasts about a week.




