Pros and Cons of 18 Medical Tests
Considering any of these screenings? Know their purpose and effectiveness—and whether you're a good candidate

To assess the evidence on the benefits and risks of 18 tests, we combed through the research and talked with medical experts from leading academic centers, government agencies, and national organizations, such as the U.S. Preventive Services Task Force (USPSTF). We skipped a few, such as blood pressure, but it’s wise to have this measured every time you see a healthcare provider or more often if you’re at higher risk for hypertension.
Check with your health insurer to make sure that the screenings your doctor advises are covered; many are, notably those recommended by the USPSTF. But also be aware that you might be charged extra fees at some testing facilities.
And note that if the screening finds something suspicious, any subsequent procedure or diagnostic test may result in extra costs for you. So ask about that, too. (The screenings below appear in alphabetical order.)
Abdominal Aortic Aneurysm Screening
This one-time ultrasound looks for a bulge in the aorta, the body’s largest artery.
Why it’s done: AAAs have the potential to burst, which can cause life-threatening bleeding.
Recommended for: Men 65 to 75 who are current or former smokers. Nonsmoking men and women ages 65 to 75 who have ever smoked might consider it if they have risk factors such as a close family member who had an AAA. The USPSTF recommends against screening nonsmoking women ages 65 to 75, whose risk is very low.
Possible outcomes: If a small AAA is found (less than 2 inches in diameter), your doctor will monitor it closely. AAAs that are larger or growing quickly may need surgical repair.
Blood Chemistry Screening
A complete blood count (CBC) measures components of your blood, such as red and white blood cells; a metabolic panel checks levels of substances such as enzymes, electrolytes, proteins, and blood sugar.
Why it’s done: To make sure levels are normal. A CBC checks for infection or conditions such as anemia. A metabolic panel checks the functioning of organs such as kidneys and liver.
Bone Density Screening
This low-dose X-ray (called a DEXA scan) measures bone density in your hips and spine.
Why it’s done: To screen for osteopenia (low bone density) and osteoporosis (weak, brittle bones).
Recommended for: Most women at age 65, but earlier—around menopause—for women with osteoporosis risk factors such as a family history or smoking, the USPSTF says. For men, consider screening at about 80, or sooner if at higher risk for fractures (due to factors such as smoking and long-term steroid use).
Possible outcomes: For osteopenia, exercise and a diet rich in vitamin D and calcium is generally advised. Rescreen in three to five years. If the scan detects osteoporosis, you may need medication to prevent fractures, and rescreening in two years. If results are normal, repeat the test in 10 years.
Carotid Artery Screening
This is an ultrasound of the artery on each side of your neck.
Why it’s done: Artery narrowing can lead to a higher stroke risk.
Recommended for: Anyone with symptoms of a stroke or ministroke. People without symptoms can skip this.
Possible outcomes: If a scan suggests a blocked carotid artery, you could get follow-up tests such as an MRI to confirm. Treatment can entail medication or surgery to clear out the artery.
Severely narrowed carotid arteries are found in only about 1 percent of adults and even then rarely lead to a stroke unless there are other risk factors, such as high blood pressure.
For people without symptoms, screening can lead to false positives, and “studies show it actually winds up hurting more people than it helps,” says Alex Krist, M.D., vice chairperson of the USPSTF.
Cholesterol Screening
This blood test measures total cholesterol levels, including LDL (bad) cholesterol, HDL (good) cholesterol, and triglycerides (artery-clogging fatty acids).
Why it’s done: Unhealthy levels—particularly total cholesterol above 240 mg/dL and LDL above 190 mg/dL—increase heart disease and stroke risks.
Recommended for: Adults ages 40 to 75 with one or more cardiovascular disease risk factors, such as smoking, high blood pressure, and diabetes, should be tested every five years, and more often if results are outside the healthy range, according to the USPSTF.
“It’s a good idea for people younger than 40 with heart-disease risk factors or a family history of very high cholesterol to get screened at least once,” says Pamela Douglas, M.D., a professor of research in cardiovascular disease at Duke University. Those older than 75 should talk with a doctor about whether screening makes sense based on their overall health.
Possible outcomes: Test results, along with other heart risk factors, may help your doctor determine whether you may benefit from medication.
Colorectal Cancer Screening
Your healthcare provider may prescribe a take-home kit; you send a stool smear to be checked for hidden blood or DNA markers for cancer. But the gold standard is a colonoscopy, an outpatient procedure that typically involves a sedative. A gastroenterologist uses a tube with a small camera attached to examine the inside of your colon. Sigmoidoscopy, which examines only the lower third of the colon, and CT colonoscopy, which uses multiple X-rays to image the colon, are used less often.
Why it’s done: To detect colon polyps, which can become cancerous.
Recommended for: Generally starting at age 50, although the American Cancer Society (ACS), citing an increase in colorectal cancer in younger people, recently recommended a first screening at age 45.
“If you are worried about colorectal cancer or you’re at higher risk because you have family members diagnosed in their 40s and 50s, that may tip your decision in favor of screening before 50,” says Otis Brawley, M.D., the former chief medical and scientific officer of the ACS. That group’s recommendations include screening every 10 years with colonoscopy, every five years with sigmoidoscopy, or every one to three years with stool tests (depending on the type).
People ages 76 to 85 should talk with their doctor about whether screening makes sense. At 80, colonoscopy risks such as colon tears and anesthesia complications rise.
Possible outcomes: Suspicious findings on any of the less invasive screenings, including sigmoidoscopy, will usually mean you’ll be advised to have a colonoscopy.
Craig Cutler Craig Cutler
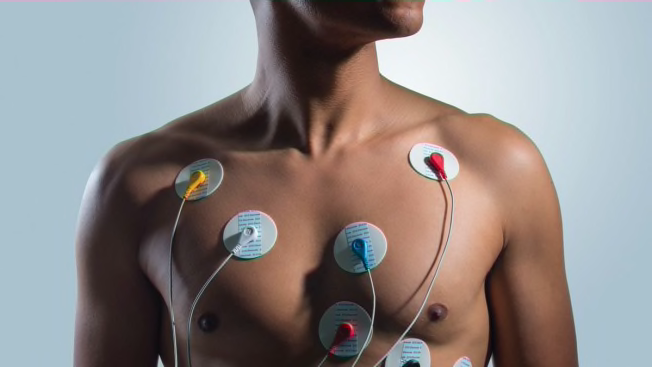
Electrocardiogram (EKG) and Exercise Stress Tests
With an EKG, electrodes attached to your chest measure your heart’s electrical activity. In an exercise stress test, you have an EKG while on a treadmill or stationary bike, or after taking medication to make your heart beat harder and faster.
Why it’s done: To check for signs of heart disease or arrhythmias.
Recommended for: Those at high risk of heart disease or those with suspected heart disease or symptoms such as chest pain or shortness of breath, as a diagnostic tool. For others, major medical groups don’t recommend the tests, which doctors sometimes do during routine physicals.
Possible outcome: For people with heart disease or symptoms, these tests may help determine the risk of a cardiac event. In low-risk people with no symptoms, they can lead to inaccurate results and unnecessary procedures, such as angiography (a heart X-ray) or angioplasty (treatment to open an artery).
Full-Body CT Scans
These use multiple X-rays to image the body and internal organs.
Why it’s done: They’re typically marketed as a way to detect early signs of cancer, heart disease, and other conditions.
Recommended for: The American Medical Association, among others, advises against these except in rare instances, and not for healthy people. Those rare cases may include people with cancer that may have spread or, in an emergency, those with a significant injury.
Possible outcomes: If the scan finds growths or abnormalities, you might need other tests and treatment. These scans often find abnormalities (an average of three per person) that almost always turn out to be harmless, according to a 2013 analysis by Air Force researchers. One-third of people have unnecessary follow-ups that expose them to additional radiation.
Heart Scans
Coronary CT angiography (CCTA) and coronary artery calcium (CAC) scans use multiple X-rays to image your arteries.
Why it’s done: Both check for plaque in arteries; a CCTA scan also looks for structural abnormalities.
Recommended for: Those with symptoms such as shortness of breath and chest pain (the CCTA), and those at risk of heart disease (the CAC). The Society of Cardiovascular Computed Tomography advises against both for most other people.
Possible outcomes: A CAC scan may help people at risk decide, with their doctor, how aggressively to treat their condition. For those with symptoms, either screening may be used with other tests to diagnose heart disease. For those at low risk, the tests expose them to radiation unnecessarily and could lead to unneeded procedures.
Mammograms and Other Breast Cancer Screenings
With a mammogram, your breast is compressed between two plates and an X-ray is taken. An increasing number of facilities use multiple X-rays to create a 3D image (called digital breast tomosynthesis). Also available are magnetic resonance imaging (MRI), which uses strong magnets and radio waves to create a detailed image of the breast, and ultrasound imaging.
Why it’s done: To detect breast cancer early, when it may be more treatable.
Recommended for: Major medical organizations agree that women should be offered the option to have a screening mammogram at age 40. The ACS advises women to start at age 45, the USPSTF recommends age 50, and the American College of Obstetricians and Gynecologists says no later than 50. Recommendations on frequency vary from one to two years. Studies suggest that 3D tests may detect slightly more cancers than standard mammograms but haven’t shown yet that they save more lives. Ultrasound imaging and an MRI can find cancers that a mammogram can miss but also pick up harmless abnormalities. These tests aren’t thought to be beneficial on their own but are useful in conjunction with mammograms for women at high risk.
Possible outcomes: These screenings may detect invasive breast cancers before they spread, sparing women more extensive treatment and possibly saving lives. But all can result in false positives, leading to unwarranted follow-up imaging and biopsies. The tests can also miss some cancers, so it’s important to talk with your doctor about your health history and risk factors, and what type of screening is best for you. There’s insufficient evidence about the effectiveness of screening after age 75.
Mouth and Neck Cancer Screening
Healthcare providers perform a physical and visual examination that may include the face, neck, nose, mouth, and throat as part of a routine exam.
Why it’s done: To check for cancers and precancers.
Recommended for: Hospitals and clinics routinely host free public screenings, but major medical organizations such as the USPSTF and ACS don’t recommend the screening for healthy people.
“There’s no clinical study showing that the exam saves lives,” says Otis Brawley, M.D. The American Dental Association does advise dentists to be alert for abnormalities during dental exams.
Possible outcomes: If anything suspicious is found, a doctor will do a biopsy and remove the lesion if it’s cancerous. Most growths found are harmless, so the exam could lead to a false positive and unnecessary biopsies and treatment.
Pap and HPV (Cervical Cancer) Tests
In a Pap test (or Pap smear) and an HPV test, your doctor removes cells from your cervix and examines them.
Why it’s done: The Pap looks for precancerous changes in cervical cells; the HPV looks for the types of human papillomavirus that cause cell changes. Both may indicate a cervical cancer risk.
Recommended for: Women ages 21 to 29 should have a Pap every three years, according to the USPSTF, ACS, and other organizations. Those 30 to 65 can follow that schedule or lengthen the time to five years if they get an HPV test at the same time.
After several normal results, you can stop screening at age 65. Women who’ve had a hysterectomy that included removal of their cervix and have never had cervical cancer or high-grade precancerous lesions don’t need screening.
Possible outcomes: Your doctor may biopsy abnormal cells and, if necessary, destroy them with a laser or extreme cold, or remove them surgically. These tests may lead to unnecessary treatment for women with false positives, notably when screenings don’t follow the recommendations. Testing for women younger than 21 is more likely to pick up harmless and temporary cell changes than potentially harmful ones.
Prostate Cancer (PSA) Test
This blood test checks for elevated levels of the prostate-specific antigen (PSA) protein produced in the prostate.
Why it’s done: High levels may be caused by prostate cancer.
Recommended for: Those who’ve already been diagnosed with prostate cancer, to help doctors monitor them. Men in their 50s and 60s might consider the test after discussing the risks and benefits with their doctor, according to guidelines from the ACS, ACP, and USPSTF. Exactly when differs from organization to organization. The ACS also recommends that men at higher risk—such as African-Americans—consider earlier screening. Men 70 and older shouldn’t be screened, according to the USPSTF, because the risks outweigh the potential benefits.
Possible outcomes: Radiation or prostate-removal surgery for those who require treatment. The test, however, often flags noncancerous conditions such as an enlarged prostate or nonaggressive cancers.
“Men should understand before they have the test that there’s a chance they may be diagnosed with a cancer that should just be watched, rather than treated,” says Brawley.
Craig Cutler Craig Cutler
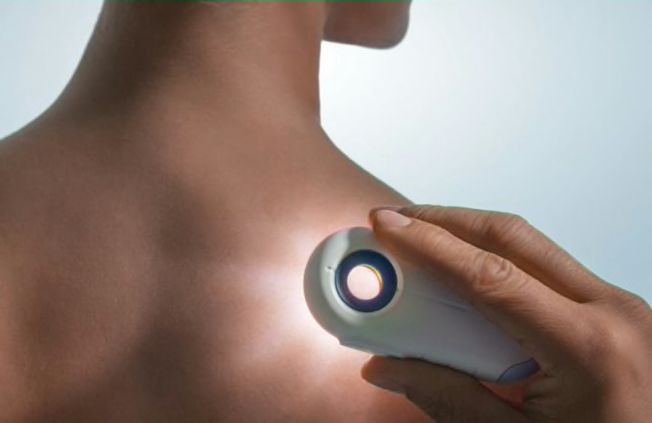
Skin Cancer Screening
A healthcare provider inspects your skin visually.
Why it’s done: For indications of skin cancer. Rates of melanoma, the most deadly skin cancer, have been rising for 30 years.
Recommended for: People at increased risk—men older than 50 and people who have more than 50 moles; those with large, unusual moles, fair skin, or reduced immunity; or those with a personal or strong family history of skin cancer—should be screened, according to the American Academy of Dermatology. If you’re among them, talk with a dermatologist about the frequency.
Everyone should familiarize themselves with their blemishes, moles, and freckles, says the ACS, and see a dermatologist if they note unusual spots, including those that are changing, itching, or bleeding.
Possible outcomes: Your doctor may biopsy a suspicious spot. For diagnosed skin cancer, treatment depends on the type and extent.
Thyroid Cancer Screening
An ultrasound is used to image the butterfly-shaped gland in the front of your neck.
Why it’s done: To check for possible cancer of the thyroid.
Recommended for: Those who have risk factors such as a close family history of thyroid cancer, or radiation exposure (such as radiation therapy), or if you or your doctor notice a lump in your neck. Others can skip it, according to the USPSTF, ACS, and other organizations.
Possible outcomes: A scan can help locate a lump that might be cancerous, or, for high-risk patients, find cancers before they become large enough to be felt. Most of the time, it detects harmless nodules or nonaggressive cancers. A vast majority of thyroid cancers grow very slowly. If the scan suggests cancer and follow-up tests confirm it, talk with your doctor about whether treatment is really needed or whether watchful waiting is a good option.
Type 2 Diabetes (Blood Sugar) Screening
Two blood tests are commonly used. A fasting glucose test measures blood sugar levels after you’ve gone without calories for at least 8 hours, and an A1C test determines your average blood sugar levels over the past three months.
Why it’s done: High levels can signify diabetes. Slightly elevated levels indicate prediabetes, increasing your risk of the full-blown disease.
Recommended for: People younger than 45 who are overweight and have at least one other risk factor—such as high blood pressure or cholesterol, a family history of diabetes, or a sedentary lifestyle—should be screened, according to the American Diabetes Association (ADA) and other medical organizations. If results are normal, retest every three years; for borderline high (prediabetes), every one to two years. One point of disagreement: For people 45 and older without risk factors, the ADA recommends screening but the USPSTF says it’s unnecessary. David Nathan, M.D., a professor of medicine at the Harvard Medical School and director of the Diabetes Center at Massachusetts General Hospital, suggests following the ADA’s recommendation. “Screening for diabetes is simple, safe, and inexpensive,” he notes.
Possible outcomes: If results suggest diabetes, you’ll need to retest to confirm, because many factors, including medication and stress, can affect your blood sugar. If diabetes or prediabetes is diagnosed, you’ll need to make dietary and exercise changes. For diabetes, you’ll probably need medication, too.
Hepatitis C Screening
A blood test that checks for this viral infection.
Why it’s done: Hepatitis C can linger in the body, symptomless, for years. Half of the people with it are unaware. Early detection and treatment prevent complications such as liver damage, cancer, and even death.
Recommended for: Anyone who was born between 1945 and 1965, had a blood transfusion before 1992, or used IV recreational drugs.
Possible outcomes: If you test positive, another blood test (hepatitis C virus RNA) is needed to confirm the diagnosis. The virus clears up on its own in about 15 to 25 percent of cases. For those who need it, antiviral medication cures the disease more than 90 percent of the time.
Lung Cancer Scan
This low-dose CT scan images the lungs.
Why it's done: It has been found to detect lung cancer early and prevent death among those at highest risk.
Recommended for: Adults 55 to 80 with a “30 pack-year” history (smoking a pack of cigarettes daily for 30 years or two packs for 15 years) who currently smoke or quit within the past 15 years should be screened yearly, says the U.S. Preventive Services Task Force. But fewer than 2 percent of them are tested, the American Society of Clinical Oncology notes.
Possible outcomes: If anything suspicious is found, additional screening or a lung biopsy may be necessary. Note: This screening has a very high rate of false positives. According to a 2013 USPSTF analysis, for every lung cancer death the scan prevents, 302 people without the disease test positive.
Editor's Note: This article also appeared in the January 2019 issue of Consumer Reports magazine. It has been updated to reflect the latest guidance from the American Dental Association.




