Fears of Legionella in Drinking Water Grow Amid Pandemic
The bacteria is sickening and sometimes killing Americans, with the reopening of buildings prompting fresh concerns
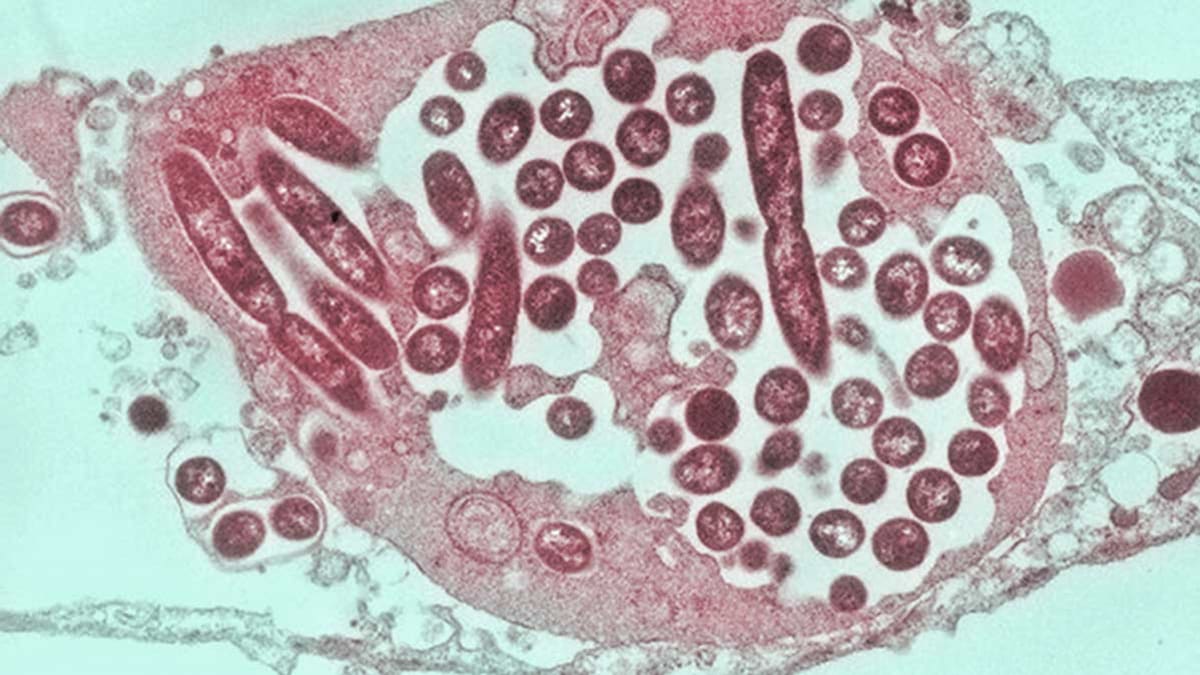
This article was co-published with Ensia, a solutions-focused nonprofit media outlet reporting on our changing planet.
Before her 73-year-old mom contracted Legionnaires’ disease at a nursing home earlier this year, Monique Barlow knew little about the deadly pneumonia and the waterborne pathogen that causes it.
“Until then, I didn’t give it much thought,” Barlow says. “I didn’t even really know what it was.”
Sheryll Barlow, a resident of Room 325 at Arlington Court Skilled Nursing and Rehab Center in suburban Columbus, Ohio, died in late February. Arlington Court was just one of at least five Columbus-area facilities to report an outbreak of Legionnaires’ disease, which is caused by Legionella bacteria, since May 2019.
Modern drinking water treatment in developed countries has effectively eliminated cholera, typhoid, and other traditional waterborne scourges. The Safe Drinking Water Act (SDWA), passed in 1974, propelled progress by requiring water suppliers to meet national standards for monitoring contaminants and managing them through filtration, disinfection, and other processes.
The U.S. now has one of the world’s safest drinking water supplies. And most of the attention on drinking water safety today has shifted from microbiological to chemical, with plastics, pesticides, and per- and polyfluoroalkyl substances, or PFAS, leading lists of contaminants of concern.
COVID-19 and Legionella
Attention to Legionella has been further heightened by the COVID-19 pandemic.
Some health experts express concern that a prior infection with the virus that causes COVID-19 could make a person more susceptible to Legionella. But there’s an even more pressing concern connecting the two: Building shutdowns through the spring and summer left warm water stagnant in pipes—a perfect environment for Legionella to multiply.
Many hotels, offices, schools, and other buildings have been left fully or partially vacant for long periods of time, notes Chris Edens, PhD, an epidemiologist with the Centers for Disease Control and Prevention, which recently released guidance for reopening buildings. “As those kinds of communities reopen, it’s important for owners and operators to be thinking about water management.”
Legionella grow naturally in the environment, especially warm freshwater lakes and streams that can be a source for drinking water. It generally becomes a risk to human health only when it enters and multiplies within human-made water and plumbing systems, and then that contaminated water becomes aerosolized.
Drinking fountains, hot tubs, sinks, toilets, sprinklers, showers, and air-conditioning systems are among the common sources. It tends to flourish when temperatures are warm, water is stagnant, chemical disinfectants are insufficient, and nutrients are plentiful, such as inside corroding pipes.
When inhaled at high enough levels, the bacteria can infiltrate the lungs and cause one of two forms of legionellosis: Pontiac fever and Legionnaires’ disease. The former is usually a fairly mild respiratory illness; the latter is far more commonly reported and estimated to be fatal in 1 in 10 cases.
Now the leading cause of reported waterborne disease in the U.S., Legionella accounts for about 60 percent of outbreaks over the last decade. Almost 10,000 cases of legionellosis were reported to the CDC in 2018—the most ever in U.S. history, and still a likely underestimate. Edens suggests the true figure is probably double that. Other scientists estimate the annual case count at between 52,000 and 70,000.
A Proliferating Pathogen
Legionnaires’ disease was discovered in 1976 after almost 200 people became ill with a mysterious type of pneumonia at an American Legion convention in Philadelphia. Dozens died. Health officials eventually identified a new bacterium that had thrived in the building’s cooling towers and then spread though the air-conditioning system.
Cooling towers were also the source of more than 2,000 confirmed cases in New York City between 2006 and 2015. In the summer of 2019, the Sheraton Atlanta hotel was closed for a month after an estimated 79 people were infected from Legionella traced to the hotel’s cooling tower and decorative fountain. The hotel chain said in a statement that it “took health and safety issues seriously,” and worked closely with relevant authorities.
A variety of other plumbing problems and insufficient water management has resulted in outbreaks around the country—at nursing homes, hospitals, and schools, and across whole communities.
At least 87 people were infected with Legionnaires’ disease in Flint, Mich., in 2014 and 2015 after the city switched water sources. Researchers found evidence for three likely sources of Legionella exposure: a hospital, city of Flint water, and local cooling towers. The mayor, Sheldon Neeley, told Ensia that the city is “making critically important infrastructure improvements to move our community forward in a positive direction.”
Yet such large-scale Legionnaires’ disease outbreaks are “just the tip of the iceberg,” according to Joan Rose, PhD, a water researcher at Michigan State University in East Lansing. Research suggests that for every case linked to a specific source and outbreak there are nine sporadic cases. For example, outbreaks accounted for only about 10 percent of the cases in New York City linked to cooling towers.
“We don’t have Legionella under control,” Rose says.


Why does Legionella appear to be on the rise around the U.S.? The answer is complicated, says Edens at the CDC. The larger numbers could be partly due to greater awareness and testing. But he suggests that an aging population and aging infrastructure are major drivers.
“In large part, our distribution system is very antiquated,” says Amy Pruden, PhD, a professor of environmental and water resources engineering at Virginia Tech in Blacksburg. As water travels through the distribution system and enters a building, it can lose disinfectant as well as interact with the materials, temperatures, and design of the building’s plumbing. “Many things are at play that affect whether these microbes grow in the plumbing,” she adds.
Climate change, too, may be playing a role. Longer summers tax the cooling devices used by large buildings. More intense storms and flooding may increase the presence of Legionella in drinking water.
It has all added up to growing concerns and heightened calls to address the risks. “The thing about Legionella is it’s a silent killer,” says Eric Hageman, a personal injury lawyer in Minneapolis who represents the family of Sheryll Barlow in a claim against Arlington Court. “You can’t see it or smell it. It’s just in the air floating around. So you have to be proactive.”
Arlington Court had been aware of a Legionella problem at the facility months before Monique Barlow’s mom became sick after another resident contracted Legionnaires’ disease in October 2019. “I just assumed they took care of everything,” Barlow says. “But then it popped back up.”
After learning that her mom had contracted the disease, she says she wanted to know more. “I felt like they owed us an explanation. How are you fixing this? How is this not going to happen again?” Barlow says.
Since Feb. 10, Arlington Court has implemented changes, including the installation of filters in the kitchen, visitor areas, showers, bathrooms, and ice machines.
Arlington Court and its parent company, Vrable, did not respond to multiple requests for comment by Ensia.
In a letter to residents, reported on March 1 after local officials announced an investigation of an outbreak, Arlington Court said it took “very seriously the health and safety of everyone at the facility.” In a statement at the time, Vrable said it was working with authorities.
Controlling Contaminants
Edens at the CDC emphasizes water management strategies, such as flushing water pipes, controlling temperatures, and using disinfectant within a building. “We know water in the tap is not sterile,” he says. “The purpose of water management is to ensure that if some Legionella bacteria come through the main, the bacteria have nowhere to grow and hide.”
Adding chlorine or other disinfectants to water as it enters a building is yet another tactic to reduce contamination.
Consumers can also take steps to reduce risks in their own households. For example, the CDC recommends that hot tub or spa owners frequently test water for proper levels of chlorine, bromine, and pH. “You need to consider the far reaches of the building,” says Cotruvo, the environmental and public health consultant. “If you’re not using a second bathroom, for example, then flush the shower before people use it.” Point-of-use water filters may also help control Legionella.
In an August 2019 report by the National Academy of Sciences, Engineering, and Medicine, a committee of 13 scientists warned that current federal, state, and local laws fail to protect the public from the spread of Legionella.
A handful of federal, state, and local regulations require certain buildings to have water management plans that include monitoring for and treatment of Legionella. But no federal law targets Legionella contamination of water supplies and building water systems.
The committee offered several recommendations for improving Legionella management in the U.S. Those include requiring a minimum disinfectant level throughout public water systems, developing clinical tools to capture more cases of Legionnaires’ disease, providing more guidance to homeowners, no longer allowing low-flow fixtures in hospitals and long-term-care facilities, addressing the longer periods of time that water sits idle, and lowering hot-water temperatures common in green buildings.
Many scientists argue a need for more urgent attention to and action on the issue.
“We need some coordination at the [federal] level,” says Pruden at Virginia Tech. “It’s a multistakeholder problem but is now awkwardly being handled through the litigation system.”
Editor’s Note: This article is a condensed version of a longer piece that you can read on Ensia’s website.
Consumer Reports has a long history of investigating America’s water. In 1974, we published a landmark three-part series (PDF) revealing that water purification systems in many communities had not kept pace with increasing levels of pollution and that many community water supplies might be contaminated. Our work helped lead to Congress enacting the Safe Drinking Water Act in December 1974.
More than 45 years later, America is still struggling with a dangerous divide between those who have access to safe and affordable drinking water and those who don’t. Communities of color often are affected disproportionately by this inequity. Consumer Reports remains committed to exposing the weaknesses in our country’s water system, including raising questions about Americans’ reliance on bottled water as an alternative—and the safety and sustainability implications of this dependence.
In addition to our ongoing investigations into bottled water, we are proud to be partnering with our readers and those of the Guardian US, another institution dedicated to journalism in the public interest, to test for dangerous contaminants in tap water samples from more than 100 communities around the country. The Guardian and CR will also be publishing related content from Ensia, a nonprofit newsroom focused on environmental issues and solutions.
America’s Water Crisis is the name we are jointly giving to this project and the series of articles we co-publish on the major challenges many in the U.S. face getting access to safe, clean, and affordable water. We will share the results of our upcoming test findings with you. In the meantime, you can join our social media conversation around water under the hashtag #waterincrisis.
Chief Content Officer, Consumer Reports




